Intraoperative Laser Speckle Contrast Imaging For Real-Time Visualization of Cerebral Blood Flow in Cerebrovascular Surgery: Results From Pre-Clinical Studies
- PMID: 32376983
- PMCID: PMC7203106
- DOI: 10.1038/s41598-020-64492-5
Intraoperative Laser Speckle Contrast Imaging For Real-Time Visualization of Cerebral Blood Flow in Cerebrovascular Surgery: Results From Pre-Clinical Studies
Abstract
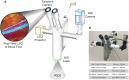
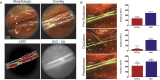
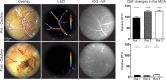
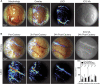
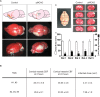
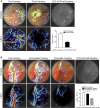
Cerebrovascular surgery can benefit from an intraoperative system that conducts continuous monitoring of cerebral blood flow (CBF). Such a system must be handy, non-invasive, and directly integrated into the surgical workflow. None of the currently available techniques, considered alone, meets all these criteria. Here, we introduce the SurgeON™ system: a newly developed non-invasive modular tool which transmits high-resolution Laser Speckle Contrast Imaging (LSCI) directly onto the eyepiece of the surgical microscope. In preclinical rodent and rabbit models, we show that this system enabled the detection of acute perfusion changes as well as the recording of temporal response patterns and degrees of flow changes in various microvascular settings, such as middle cerebral artery occlusion, femoral artery clipping, and complete or incomplete cortical vessel cautery. During these procedures, a real-time visualization of vasculature and CBF was available in high spatial resolution through the eyepiece as a direct overlay on the live morphological view of the surgical field. Upon comparison with indocyanine green angiography videoangiography (ICG-VA) imaging, also operable via SurgeON, we found that direct-LSCI can produce greater information than ICG-VA and that continuous display of data is advantageous for performing immediate LSCI-guided adjustments in real time.
Conflict of interest statement
Authors A.R., J.C., K.R., S.I.C. and M.J.B. were employed by Vasoptic Medical, Inc. when the research was carried out. A.R., K.R., M.J.B have ownership interests in Vasoptic Medical, Inc. One or more patents pertaining to the system and methods described in this manuscript are assigned to Vasoptic Medical, Inc. and list A.R. and M.J.B. as inventors.
Figures
References
-
- Zaidi, H. A. et al. Indocyanine green angiography in the surgical management of cerebral arteriovenous malformations: lessons learned in 130 consecutive cases. Neurosurgery10 Suppl 2, 246–251; discussion 251, 10.1227/neu.0000000000000318 (2014). - PubMed
-
- Dashti, R., Laakso, A., Niemela, M., Porras, M. & Hernesniemi, J. Microscope-integrated near-infrared indocyanine green videoangiography during surgery of intracranial aneurysms: the Helsinki experience. Surgical neurology71, 543–550; discussion 550, 10.1016/j.surneu.2009.01.027 (2009). - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources

