Early identification of patients with chest pain at very low risk of acute myocardial infarction using clinical information and ECG only
- PMID: 32383504
- PMCID: PMC7507208
- DOI: 10.1111/ijcp.13526
Early identification of patients with chest pain at very low risk of acute myocardial infarction using clinical information and ECG only
Abstract
Background: A considerable proportion of patients with angina-like symptoms in an emergency department have very low pretest probability for acute myocardial infarction (AMI). Numerous algorithms exist for the exclusion of AMI, usually including laboratory tests. We aimed to investigate whether patients with very low risk can safely be identified by ECG and clinical information without biomarker testing, contributing to saving time and costs.
Methods: Prospective diagnostic test accuracy study. We included all consecutive patients presenting with angina at the department of emergency medicine of a tertiary care hospital during a 1-year period. Using clinical information without biomarker testing and ECG, the "Mini-GRACE score," based on the well-established GRACE-score without using laboratory parameters was calculated. In a cohort design we compared the index test Mini-GRACE to AMI as reference standard in the final diagnosis using standard measures of diagnostic test accuracy.
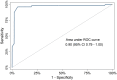
Results: We included 2755 patients (44% female, age 44 ± 17 years). AMI was diagnosed in 103 (4%) patients, among those 44% with STEMI. Overall 2562 patients (93%) had a negative "Mini-GRACE," four (0.2%) of these patients had myocardial infarction, and this results in a sensitivity of 96.1% (95% CI 90.4%-98.9%), specificity 96.5% (95.7%-97.1%), positive predictive value 51.3% (46.3%-56.3%) and negative predictive value 99.8% (99.6%-99.9%). Model performance according to C statistic (0.90) and Brier score (0.0045) was excellent. In rule-out patients 30-day mortality was 0.3% and 1-year mortality was 0.8%.
Conclusions: Patients with very low risk of AMI can be identified with high certainty using clinical information without biomarker testing and ECG. Cardiac biomarkers might be avoided in such cases, potentially leading to a significant cost reduction.
Keywords: acute coronary syndrome; emergency department; rule-out.
© 2020 The Authors. International Journal of Clinical Practice published by John Wiley & Sons Ltd.
Conflict of interest statement
All authors state that there are no potential conflicts of interest to disclose.
Figures
References
-
- Lopez AD, Mathers CD, Ezzati M, Jamison DT, Murray CJ. Global and regional burden of disease and risk factors, 2001: systematic analysis of population health data. Lancet. 2006;367:1747‐1757. - PubMed
-
- Roffi M, Patrono C, Collet JP, et al. 2015 ESC Guidelines for the management of acute coronary syndromes in patients presenting without persistent ST‐segment elevation: Task Force for the Management of Acute Coronary Syndromes in Patients Presenting without Persistent ST‐Segment Elevation of the European Society of Cardiology (ESC). Eur Heart J. 2016;37:267‐315. - PubMed
-
- Steg PG, James SK, Atar D, et al. ESC Guidelines for the management of acute myocardial infarction in patients presenting with ST‐segment elevation. Eur Heart J. 2012;33:2569‐2619. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical