Anti-inflammatory properties of uvaol on DSS-induced colitis and LPS-stimulated macrophages
- PMID: 32411289
- PMCID: PMC7206718
- DOI: 10.1186/s13020-020-00322-0
Anti-inflammatory properties of uvaol on DSS-induced colitis and LPS-stimulated macrophages
Abstract
Background: Apocynum venetum leaves are used as a kind of phytomedicine and the main ingredient in some traditional Chinese medicine products for the relief of colitis. To understand the bioactive constituents of A. venetum L., we did a phytochemistry study and investigated anti-Inflammatory effects of compounds and explored the underlying mechanisms.
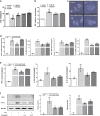
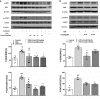
Methods: We isolated compounds from ethanol extract of A. venetum L. leaf and detected the most effective compound by NO inhibition assay. We investigated anti-Inflammatory effects on dextran sulfate sodium (DSS)-induced colitis mice and lipopolysaccharide (LPS)-stimulated RAW264.7 cells. The disease activity index was determined by scores of body weight loss, diarrhea and rectal bleeding; histological damage was analyzed by H&E staining; macrophages change in the colon were analyzed by immunohistochemistry (IHC); myeloperoxidase activity was measured by myeloperoxidase assay kits; levels of proinflammatory cytokines were determined by qPCR and ELISA; protein production such as COX-2, iNOS, STAT3 and ERK1/2 were determined by western blotting.
Results: We isolated uvaol from ethanol extract of A. venetum L. leaf and found uvaol has excellent potential of inhibiting NO production. We further found uvaol could attenuate disease activity index (DAI), colon shortening, colon injury, and colonic myeloperoxidase activity in DSS-induced colitis mice. Moreover, uvaol significantly reduces mRNA expression and production of pro-inflammatory cytokines (TNF-α, IL-6, IL-1β, and MCP-1) and infiltration of macrophages in colonic tissues of colitis mice. Studies on LPS challenged murine macrophage RAW246.7 cells also revealed that uvaol reduces mRNA expression and production of pro-inflammatory cytokines and mediators. Mechanically, uvaol inhibits the pro-inflammatory ERK/STAT3 axis in both inflamed colonic tissues and macrophages.
Conclusions: A. venetum leaf contains uvaol and uvaol has potent anti-inflammatory effects on DSS-induced experimental colitis and LPS-stimulated RAW264.7 macrophage cells. These results suggest uvaol is a prospective anti-inflammatory agent for colonic inflammation.
Keywords: Anti-inflammatory; Apocynum venetum L.; Colonic inflammation; Macrophage; Uvaol.
© The Author(s) 2020.
Conflict of interest statement
Competing interestsThe authors declare that they have no competing interests.
Figures




Similar articles
-
Qing-dai powder promotes recovery of colitis by inhibiting inflammatory responses of colonic macrophages in dextran sulfate sodium-treated mice.Chin Med. 2015 Oct 13;10:29. doi: 10.1186/s13020-015-0061-x. eCollection 2015. Chin Med. 2015. PMID: 26464580 Free PMC article.
-
Canna x generalis L.H. Bailey rhizome extract ameliorates dextran sulfate sodium-induced colitis via modulating intestinal mucosal dysfunction, oxidative stress, inflammation, and TLR4/ NF-ҡB and NLRP3 inflammasome pathways.J Ethnopharmacol. 2021 Apr 6;269:113670. doi: 10.1016/j.jep.2020.113670. Epub 2020 Dec 8. J Ethnopharmacol. 2021. PMID: 33301917
-
Safranal Alleviates Dextran Sulfate Sodium-Induced Colitis and Suppresses Macrophage-Mediated Inflammation.Front Pharmacol. 2019 Nov 1;10:1281. doi: 10.3389/fphar.2019.01281. eCollection 2019. Front Pharmacol. 2019. PMID: 31736758 Free PMC article.
-
Artemisinin analogue SM934 ameliorates DSS-induced mouse ulcerative colitis via suppressing neutrophils and macrophages.Acta Pharmacol Sin. 2018 Oct;39(10):1633-1644. doi: 10.1038/aps.2017.185. Epub 2018 May 31. Acta Pharmacol Sin. 2018. PMID: 29849131 Free PMC article.
-
Apocynum venetum, a medicinal, economical and ecological plant: a review update.PeerJ. 2023 Mar 7;11:e14966. doi: 10.7717/peerj.14966. eCollection 2023. PeerJ. 2023. PMID: 36908824 Free PMC article. Review.
Cited by
-
Luminescent Nanocomposite SiO2/EuTTA/ZIF‑8 Loaded with Uvaol: Synthesis, Characterization, Anti-Inflammatory Effects, and Molecular Docking Analysis.ACS Omega. 2025 Jul 14;10(29):32391-32403. doi: 10.1021/acsomega.5c04682. eCollection 2025 Jul 29. ACS Omega. 2025. PMID: 40757268 Free PMC article.
-
Activation of P2Y1R impedes intestinal mucosa repair during colitis.Int J Biol Sci. 2023 Aug 21;19(14):4360-4375. doi: 10.7150/ijbs.82302. eCollection 2023. Int J Biol Sci. 2023. PMID: 37781034 Free PMC article.
-
Selected Medicinal Plants Used in the Treatment and Management of Tuberculosis and Related Symptoms in South Africa.Pharmaceuticals (Basel). 2025 Mar 31;18(4):513. doi: 10.3390/ph18040513. Pharmaceuticals (Basel). 2025. PMID: 40283948 Free PMC article. Review.
-
Total Flavonoids Extracts of Apocynum L. from the Ili River Valley Region at Different Harvesting Periods and Bioactivity Analysis.Molecules. 2022 Oct 28;27(21):7343. doi: 10.3390/molecules27217343. Molecules. 2022. PMID: 36364168 Free PMC article.
-
Network Pharmacology Study of Bioactive Components and Molecular Mechanisms of the Glycoside Fraction from Picrorhiza scrophulariiflora Against Experimental Colitis.Drug Des Devel Ther. 2023 May 23;17:1531-1546. doi: 10.2147/DDDT.S407339. eCollection 2023. Drug Des Devel Ther. 2023. PMID: 37249930 Free PMC article.
References
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

