Pharmacological management of modifiable cardiovascular risk factors (blood pressure and lipids) following diagnosis of myocardial infarction, stroke and diabetes: comparison between population-based studies in Russia and Norway
- PMID: 32430002
- PMCID: PMC7236339
- DOI: 10.1186/s12872-020-01513-1
Pharmacological management of modifiable cardiovascular risk factors (blood pressure and lipids) following diagnosis of myocardial infarction, stroke and diabetes: comparison between population-based studies in Russia and Norway
Abstract
Background: Cardiovascular disease (CVD) mortality is substantially higher in Russia than in neighbouring Norway. We aimed to compare blood pressure- and lipid-lowering medication use and proportion meeting treatment targets between general population samples in the two countries in those with CVD and diabetes.
Methods: The study population was adults aged 40-69 years reporting a diagnosis of myocardial infarction (MI), stroke and/or diabetes participating in cross-sectional population-based studies in Russia (Know Your Heart (KYH) 2015-18 N = 626) and Norway (The Tromsø Study 2015-16 (Tromsø 7) N = 1353). Reported medications were coded according to the 2016 WHO Anatomical Therapeutic Chemical Classification system. Treatment targets were defined using the Joint European Societies guidelines for CVD prevention in clinical practice (2016).
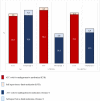
Results: Age- and sex-standardized prevalence of use of lipid-lowering medications was higher in Tromsø 7 for all three conditions with a disproportionately large difference in those reporting MI (+ 48% (95% CI 39, 57%)). Proportion meeting treatment targets for LDL cholesterol was poor in both studies (age- and sex-standardized prevalence of control KYH vs Tromsø 7: MI 5.1% vs 10.1%; stroke 11.6% vs 5.8%; diabetes 24.9% vs 23.3%). Use of antihypertensive medication was higher in KYH for stroke (+ 40% (95% CI 30, 50%)) and diabetes (+ 27% (95% CI 19, 34%)) groups but approximately equal for the MI group (- 1% (95% CI -1, 1%)). Proportion meeting blood pressure targets was lower in KYH vs Tromsø 7 (MI 51.8% vs 76.3%; stroke 49.5% vs 69.6%; diabetes 51.9% vs 63.9%).
Conclusions: We identified different patterns of medication use in people with CVD and diabetes. However despite higher use of lipid-lowering medication in the Norwegian study treatment to target for total cholesterol was poor in both Russian and Norwegian studies. In contrast we found higher levels of use of antihypertensive medications in the Russian study but also that less participants met treatment targets for blood pressure. Further work should investigate what factors are responsible for this seeming paradox and how management of modifiable risk factors for secondary prevention could be improved.
Keywords: Diabetes; Myocardial infarction; Norway; Russian Federation; Secondary prevention; Stroke.
Conflict of interest statement
Henrik Schirmer has received an unrestricted research grant from Astra Zeneca and lecture fees from Astra Zeneca, MSD, Novartis and Sanofi Aventis.
Figures

Similar articles
-
Uncontrolled and apparent treatment resistant hypertension: a cross-sectional study of Russian and Norwegian 40-69 year olds.BMC Cardiovasc Disord. 2020 Mar 13;20(1):135. doi: 10.1186/s12872-020-01407-2. BMC Cardiovasc Disord. 2020. PMID: 32169049 Free PMC article.
-
Risk Factor Control in Stroke Survivors with Diagnosed and Undiagnosed Diabetes: A Ghanaian Registry Analysis.J Stroke Cerebrovasc Dis. 2020 Dec;29(12):105304. doi: 10.1016/j.jstrokecerebrovasdis.2020.105304. Epub 2020 Sep 22. J Stroke Cerebrovasc Dis. 2020. PMID: 32992189
-
Pharmacological treatment of hypertension and hyperlipidemia in Izhevsk, Russia.BMC Cardiovasc Disord. 2016 Jun 3;16:122. doi: 10.1186/s12872-016-0300-9. BMC Cardiovasc Disord. 2016. PMID: 27255373 Free PMC article.
-
Single Pill Regimen Leads to Better Adherence and Clinical Outcome in Daily Practice in Patients Suffering from Hypertension and/or Dyslipidemia: Results of a Meta-Analysis.High Blood Press Cardiovasc Prev. 2020 Apr;27(2):157-164. doi: 10.1007/s40292-020-00370-5. Epub 2020 Mar 26. High Blood Press Cardiovasc Prev. 2020. PMID: 32219670 Free PMC article. Review.
-
Antiplatelet activity of drugs used in hypertension, dyslipidemia and diabetes: Additional benefit in cardiovascular diseases prevention.Vascul Pharmacol. 2017 Apr;91:10-17. doi: 10.1016/j.vph.2017.03.004. Epub 2017 Mar 22. Vascul Pharmacol. 2017. PMID: 28342822 Review.
Cited by
-
Awareness of Hypertension, Hypercholesterolemia, and Diabetes Mellitus and Associated Characteristics in Russian Adults.Int J Hypertens. 2024 Mar 25;2024:8542671. doi: 10.1155/2024/8542671. eCollection 2024. Int J Hypertens. 2024. PMID: 38567246 Free PMC article.
References
-
- Global Health Observatory. World Health Organisation. Total NCD Mortality Data by country Geneva: Available online http://apps.who.int/gho/data/node.main. A860?lang=en 2017 [.
-
- World Health Organisation. WHO Mortality Database. Available online http://www.who.int/healthinfo/mortality_data/en/ access date 07/12/2017; 2017.
-
- Kotseva K, Wood D, De Bacquer D, De Backer G, Ryden L, Jennings C, et al. EUROASPIRE IV: a European Society of Cardiology survey on the lifestyle, risk factor and therapeutic management of coronary patients from 24 European countries. Eur J Prev Cardiol. 2016;23(6):636–648. doi: 10.1177/2047487315569401. - DOI - PubMed
-
- Piepoli MF, Hoes AW, Agewall S, Albus C, Brotons C, Catapano AL, et al. 2016 European Guidelines on cardiovascular disease prevention in clinical practice: The Sixth Joint Task Force of the European Society of Cardiology and Other Societies on Cardiovascular Disease Prevention in Clinical Practice (constituted by representatives of 10 societies and by invited experts) Developed with the special contribution of the European Association for Cardiovascular Prevention & Rehabilitation (EACPR) Eur Heart J. 2016;37(29):2315–2381. doi: 10.1093/eurheartj/ehw106. - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

