The Association Between Neighborhood Socioeconomic Disadvantage and Chronic Obstructive Pulmonary Disease
- PMID: 32440110
- PMCID: PMC7211318
- DOI: 10.2147/COPD.S238933
The Association Between Neighborhood Socioeconomic Disadvantage and Chronic Obstructive Pulmonary Disease
Abstract
Rationale: Individual socioeconomic status has been shown to influence the outcomes of patients with chronic obstructive pulmonary disease (COPD). However, contextual factors may also play a role. The objective of this study is to evaluate the association between neighborhood socioeconomic disadvantage measured by the area deprivation index (ADI) and COPD-related outcomes.
Methods: Residential addresses of SubPopulations and InteRmediate Outcome Measures in COPD Study (SPIROMICS) subjects with COPD (FEV1/FVC <0.70) at baseline were geocoded and linked to their respective ADI national ranking score at the census block group level. The associations between the ADI and COPD-related outcomes were evaluated by examining the contrast between participants living in the most-disadvantaged (top quintile) to the least-disadvantaged (bottom quintile) neighborhood. Regression models included adjustment for individual-level demographics, socioeconomic variables (personal income, education), exposures (smoking status, packs per year, occupational exposures), clinical characteristics (FEV1% predicted, body mass index) and neighborhood rural status.
Results: A total of 1800 participants were included in the analysis. Participants residing in the most-disadvantaged neighborhoods had 56% higher rate of COPD exacerbation (P<0.001), 98% higher rate of severe COPD exacerbation (P=0.001), a 1.6 point higher CAT score (P<0.001), 3.1 points higher SGRQ (P<0.001), and 24.6 meters less six-minute walk distance (P=0.008) compared with participants who resided in the least disadvantaged neighborhoods.
Conclusion: Participants with COPD who reside in more-disadvantaged neighborhoods had worse COPD outcomes compared to those residing in less-disadvantaged neighborhoods. Neighborhood effects were independent of individual-level socioeconomic factors, suggesting that contextual factors could be used to inform intervention strategies targeting high-risk persons with COPD.
Keywords: COPD; area deprivation index; health disparities.
© 2020 Galiatsatos et al.
Conflict of interest statement
Dr Laura Paulin reports grants from NIEHS, during the conduct of the study. Dr Nirupama Putcha reports grants from NIH, outside the submitted work. Dr Christopher Cooper reports personal fees from GlaxoSmithKline, outside the submitted work. Dr Mark Dransfield reports grants from NIH, during the conduct of the study. Dr R Graham Barr reports grants from NIH, Foundation for the NIH, grants, non-financial support from COPD Foundation, during the conduct of the study. Dr Alejandro Comellas reports grants from NIH, during the conduct of the study; non-financial support from VIDA, outside the submitted work. Dr Meilan Han reports personal fees from GSK, AZ, BI, Merck, and Mylan, non-financial support from Novartis, grants from Sunovion, outside the submitted work. Professor Stephen Peters reports grants from NIH and NHLBI, outside the submitted work. Dr Jerry Krishnan reports grants from NIH and ResMed, during the conduct of the study. Dr Wassim Labaki reports non-financial support from Pulmonx, outside the submitted work. Dr Meredith McCormack reports grants from NIH/NIMHD and Environmental Protection Agency, during the conduct of the study; personal fees from Celgene, Glaxo Smith Kline, and UpToDate, outside the submitted work. Dr Nadia Hansel reports grants, personal fees from AstraZeneca and GSK, grants from Boehringer Ingelheim and COPD Foundation, and NIH; personal fees from Mylan, outside the submitted work. The authors report no other conflicts of interest in this work.
Figures
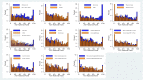

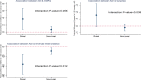
References
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Molecular Biology Databases
Miscellaneous

