A proposed lung ultrasound and phenotypic algorithm for the care of COVID-19 patients with acute respiratory failure
- PMID: 32440906
- PMCID: PMC7241588
- DOI: 10.1007/s12630-020-01704-6
A proposed lung ultrasound and phenotypic algorithm for the care of COVID-19 patients with acute respiratory failure
Abstract
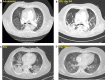
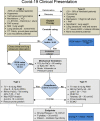
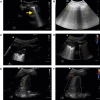
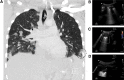
Pulmonary complications are the most common clinical manifestations of coronavirus disease (COVID-19). From recent clinical observation, two phenotypes have emerged: a low elastance or L-type and a high elastance or H-type. Clinical presentation, pathophysiology, pulmonary mechanics, radiological and ultrasound findings of these two phenotypes are different. Consequently, the therapeutic approach also varies between the two. We propose a management algorithm that combines the respiratory rate and oxygenation index with bedside lung ultrasound examination and monitoring that could help determine earlier the requirement for intubation and other surveillance of COVID-19 patients with respiratory failure.
RéSUMé: Les complications pulmonaires du coronavirus (COVID-19) constituent ses manifestations cliniques les plus fréquentes. De récentes observations cliniques ont fait émerger deux phénotypes : le phénotype à élastance faible ou type L (low), et le phénotype à élastance élevée, ou type H (high). La présentation clinique, la physiopathologie, les mécanismes pulmonaires, ainsi que les observations radiologiques et échographiques de ces deux différents phénotypes sont différents. L’approche thérapeutique variera par conséquent selon le phénotype des patients atteints de COVID-19 souffrant d’insuffisance respiratoire.
Keywords: COVID-19; and oxygenation index; lung ultrasound; respiratory failure; respiratory rate.
Figures
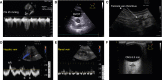
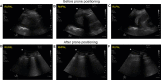
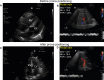
Similar articles
-
Lung Ultrasound in Patients with Acute Respiratory Failure Reduces Conventional Imaging and Health Care Provider Exposure to COVID-19.Ultrasound Med Biol. 2020 Aug;46(8):2090-2093. doi: 10.1016/j.ultrasmedbio.2020.04.033. Epub 2020 May 6. Ultrasound Med Biol. 2020. PMID: 32451194 Free PMC article.
-
Pathophysiological background and clinical practice of lung ultrasound in COVID-19 patients: A short review.Anatol J Cardiol. 2020 Aug;24(2):76-80. doi: 10.14744/AnatolJCardiol.2020.33645. Anatol J Cardiol. 2020. PMID: 32749247 Free PMC article. Review.
-
Lung ultrasound for early diagnosis and severity assessment of pneumonia in patients with coronavirus disease 2019.Korean J Intern Med. 2020 Jul;35(4):771-781. doi: 10.3904/kjim.2020.180. Epub 2020 Jul 1. Korean J Intern Med. 2020. PMID: 32668514 Free PMC article.
-
Point-of-care lung ultrasound in three neonates with COVID-19.Eur J Pediatr. 2020 Aug;179(8):1279-1285. doi: 10.1007/s00431-020-03706-4. Epub 2020 Jun 5. Eur J Pediatr. 2020. PMID: 32504135 Free PMC article.
-
Supportive Management and Interventions for Respiratory Failure Due to SARS-CoV-2.Crit Care Nurs Q. 2020 Oct/Dec;43(4):369-380. doi: 10.1097/CNQ.0000000000000322. Crit Care Nurs Q. 2020. PMID: 32833773 Review.
Cited by
-
Thoracic imaging outcomes in COVID-19 survivors.World J Radiol. 2021 Jun 28;13(6):149-156. doi: 10.4329/wjr.v13.i6.149. World J Radiol. 2021. PMID: 34249236 Free PMC article. Review.
-
Lung Ultrasound in Critical Care: A Narrative Review.Diagnostics (Basel). 2025 Mar 17;15(6):755. doi: 10.3390/diagnostics15060755. Diagnostics (Basel). 2025. PMID: 40150097 Free PMC article. Review.
-
Chest physiotherapy: An important adjuvant in critically ill mechanically ventilated patients with COVID-19.Respir Physiol Neurobiol. 2020 Nov;282:103529. doi: 10.1016/j.resp.2020.103529. Epub 2020 Aug 17. Respir Physiol Neurobiol. 2020. PMID: 32818606 Free PMC article. Review.
-
A physiological approach to understand the role of respiratory effort in the progression of lung injury in SARS-CoV-2 infection.Crit Care. 2020 Aug 10;24(1):494. doi: 10.1186/s13054-020-03197-7. Crit Care. 2020. PMID: 32778136 Free PMC article. Review.
-
Three Zone Scanning Protocol For Lung Ultrasound: An Anatomical Basis.Heart Lung Circ. 2023 Feb;32(2):247-251. doi: 10.1016/j.hlc.2022.09.013. Epub 2022 Nov 16. Heart Lung Circ. 2023. PMID: 36400698 Free PMC article.
References
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

