Risk of Graft Failure in Kidney Recipients with Cured Post-Transplant Cancer
- PMID: 32449324
- PMCID: PMC7246187
- DOI: 10.3346/jkms.2020.35.e166
Risk of Graft Failure in Kidney Recipients with Cured Post-Transplant Cancer
Abstract
Background: Post-transplant cancer (PTC) is a critical complication after kidney transplantation. However, whether successfully cured PTC affects the long-term graft outcome remains unclear.
Methods: We retrospectively reviewed 1,629 kidney transplant recipients from 1995 to 2017 after excluding patients with post-transplant hematologic or advanced non-curable cancers and who underwent allograft nephrectomy because of cancer. Cured PTCs were defined as cancers treated with curative methods and/or adjuvant therapy without recurrence during ≥ 2 years. Propensity score matching was performed to match cured PTC patients with cancer-naïve patients (i.e., non-PTC group).
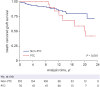
Results: During the median period of 7 years (maximum, 23 years), 70 patients (4.3%) had cured PTCs. The PTC group showed significantly higher risks of death-censored graft failure (adjusted hazard ratio [HR], 2.56 [1.05-6.23]), class II donor-specific antibodies (adjusted HRs, 3.37 [1.30-8.71]), estimated glomerular filtration rate < 30 mL/min/1.73 m² (adjusted HR, 2.68 [1.43-5.02]) and random urine protein/creatinine ratio > 1 g (adjusted HR, 3.61 [1.92-6.79]) compared to non-PTC group. However, the risk of mortality was not different between the PTC and non-PTC groups. According to the cancer type, only urogenital cancer had a significant association with graft failure (adjusted HR, 4.26 [1.19-15.22]) and the gastrointestinal cancer showed elevated risk of T cell mediated rejection compared to non-PTC (adjusted HR, 20.44 [6.02-69.39]).
Conclusion: Appropriate monitoring of graft function is necessary in patients with cured PTCs.
Keywords: Cancer; Graft Function; Kidney Transplantation; Malignancy; Mortality.
© 2020 The Korean Academy of Medical Sciences.
Conflict of interest statement
The authors have no potential conflicts of interest to disclose.
Figures

Similar articles
-
Risk Factors Affecting Graft and Patient Survivals After Transplantation From Deceased Donors in a Developing Country: A Single-Center Experience.Transplant Proc. 2017 Mar;49(2):270-277. doi: 10.1016/j.transproceed.2016.12.009. Transplant Proc. 2017. PMID: 28219583
-
Peritubular capillary C4d staining in late acute renal allograft rejection--is it relevant?Clin Transplant. 2008 Jan-Feb;22(1):61-7. doi: 10.1111/j.1399-0012.2007.00745.x. Clin Transplant. 2008. PMID: 18217907
-
Effect of BMI on allograft function and survival in pediatric renal transplant recipients.Pediatr Nephrol. 2018 Aug;33(8):1429-1435. doi: 10.1007/s00467-018-3942-2. Epub 2018 Mar 25. Pediatr Nephrol. 2018. PMID: 29574612
-
Peritubular capillary C4d deposition and renal outcome in post-transplant IgA nephropathy.Clin Transplant. 2007 Mar-Apr;21(2):159-65. doi: 10.1111/j.1399-0012.2007.00487.x. Clin Transplant. 2007. PMID: 17425739 Review.
-
Managing immunosuppressive therapy in potentially cured post-kidney transplant cancer (excluding non-melanoma skin cancer): an overview of the available evidence and guidance for shared decision-making.Transpl Int. 2021 Oct;34(10):1789-1800. doi: 10.1111/tri.13952. Transpl Int. 2021. PMID: 34146426 Free PMC article. Review.
Cited by
-
Comorbid Conditions in Kidney Transplantation: Outcome Analysis at King Abdulaziz Medical City.Cureus. 2023 Jul 4;15(7):e41355. doi: 10.7759/cureus.41355. eCollection 2023 Jul. Cureus. 2023. PMID: 37546132 Free PMC article.
References
-
- Israni AK, Snyder JJ, Skeans MA, Peng Y, Maclean JR, Weinhandl ED, et al. Predicting coronary heart disease after kidney transplantation: Patient Outcomes in Renal Transplantation (PORT) study. Am J Transplant. 2010;10(2):338–353. - PubMed
-
- Porrini EL, Díaz JM, Moreso F, Delgado Mallén PI, Silva Torres I, Ibernon M, et al. Clinical evolution of post-transplant diabetes mellitus. Nephrol Dial Transplant. 2016;31(3):495–505. - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

