Orthostatic Blood Pressure Recovery Is Associated With the Rate of Cognitive Decline and Mortality in Clinical Alzheimer's Disease
- PMID: 32449919
- PMCID: PMC7566323
- DOI: 10.1093/gerona/glaa129
Orthostatic Blood Pressure Recovery Is Associated With the Rate of Cognitive Decline and Mortality in Clinical Alzheimer's Disease
Abstract
Background: Impaired recovery of blood pressure (BP) after standing has been shown to be related to cognitive function and mortality in people without dementia, but its role in people with Alzheimer's disease (AD) is unknown. The aim of this study was to investigate the association of the orthostatic BP response with cognitive decline and mortality in AD.
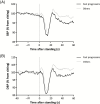
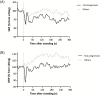
Methods: In this post hoc analysis of a randomized controlled trial (Nilvad), we measured the beat-to-beat response of BP upon active standing in mild-to-moderate AD. This included the initial drop (nadir within 40 seconds) and recovery after 1 minute, both expressed relative to resting values. We examined the relationship between a small or large initial drop (median split) and unimpaired (≥100%) or impaired recovery (<100%) with 1.5-year change in Alzheimer's Disease Assessment-cognitive subscale (ADAS-cog) scores and all-cause mortality.
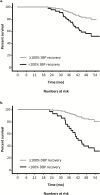
Results: We included 55 participants (age 73.1 ± 6.2 years). Impaired BP recovery was associated with higher increases in ADAS-cog scores (systolic: β [95% confidence interval] = 5.6 [0.4-10.8], p = .035; diastolic: 7.6 [2.3-13.0], p = .006). During a median follow-up time of 49 months, 20 participants died. Impaired BP recovery was associated with increased mortality (systolic: HR [95% confidence interval] = 2.9 [1.1-7.8], p = .039; diastolic: HR [95% confidence interval] = 5.5 [1.9-16.1], p = .002). The initial BP drop was not associated with any outcome. Results were adjusted for age, sex, and intervention group.
Conclusions: Failure to fully recover BP after 1 minute of standing is associated with cognitive decline and mortality in AD. As such, BP recovery can be regarded as an easily obtained marker of progression rate of AD.
Keywords: Alzheimer’s disease; Blood pressure; Continuous monitoring; Dementia; Resilience.
© The Author(s) 2020. Published by Oxford University Press on behalf of The Gerontological Society of America.
Figures
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials

