Molecular Basis of Bone Aging
- PMID: 32456199
- PMCID: PMC7279376
- DOI: 10.3390/ijms21103679
Molecular Basis of Bone Aging
Abstract
A decline in bone mass leading to an increased fracture risk is a common feature of age-related bone changes. The mechanisms underlying bone senescence are very complex and implicate systemic and local factors and are the result of the combination of several changes occurring at the cellular, tissue and structural levels; they include alterations of bone cell differentiation and activity, oxidative stress, genetic damage and the altered responses of bone cells to various biological signals and to mechanical loading. The molecular mechanisms responsible for these changes remain greatly unclear and many data derived from in vitro or animal studies appear to be conflicting and heterogeneous, probably due to the different experimental approaches; nevertheless, understanding the main physio-pathological processes that cause bone senescence is essential for the development of new potential therapeutic options for treating age-related bone loss. This article reviews the current knowledge concerning the molecular mechanisms underlying the pathogenesis of age-related bone changes.
Keywords: bone aging; bone loss; osteoporosis; senescence.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

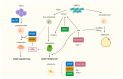
References
-
- Sheer R.L., Barron R.L., Sudharshan L., Pasquale M.K. Validated prediction of imminent risk of fracture for older adults. Am. J. Manag. Care. 2020;26:e91–e97. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

