Impact of Circadian Blood Pressure Pattern on Silent Cerebral Small Vessel Disease: A Systematic Review and Meta-Analysis
- PMID: 32476573
- PMCID: PMC7429026
- DOI: 10.1161/JAHA.119.016299
Impact of Circadian Blood Pressure Pattern on Silent Cerebral Small Vessel Disease: A Systematic Review and Meta-Analysis
Abstract
Background Abnormal circadian blood pressure (BP) variations during sleep, specifically the non-dipping (<10% fall in nocturnal BP) and reverse-dipping patterns (rise in nocturnal BP), have been associated with an increased risk of cardiovascular events and target organ damage. However, the relationship between abnormal sleep BP variations and cerebral small vessel disease markers is poorly established. This study aims to assess the association between non-dipping and reverse-dipping BP patterns with markers of silent cerebral small vessel disease. Methods and Results MEDLINE, Embase, and Cochrane Databases were searched from inception through November 2019. Studies that reported the odds ratios (ORs) for cerebral small vessel disease markers in patients with non-dipping or reverse-dipping BP patterns were included. Effect estimates from the individual studies were extracted and combined using the random-effect, generic inverse variance method of DerSimonian and Laird. Twelve observational studies composed of 3497 patients were included in this analysis. The reverse-dipping compared with normal dipping BP pattern was associated with a higher prevalence of white matter hyperintensity with a pooled adjusted OR of 2.00 (95% CI, 1.13-2.37; I2=36%). Non-dipping BP pattern compared with normal dipping BP pattern was associated with higher prevalence of white matter hyperintensity and asymptomatic lacunar infarction, with pooled ORs of 1.38 (95% CI, 0.95-2.02; I2=52%) and 2.33 (95% CI, 1.30-4.18; I2=73%), respectively. Limiting to only studies with confounder-adjusted analysis resulted in a pooled OR of 1.38 (95% CI, 0.95-2.02; I2=52%) for white matter hyperintensity and 1.44 (95% CI, 0.97-2.13; I2=0%) for asymptomatic lacunar infarction. Conclusions The non-dipping and reverse-dipping BP patterns are associated with neuroimaging cerebral small vessel disease markers.
Keywords: blood pressure variability; circadian; meta‐analysis; microbleed; white matter.
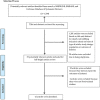
Figures


References
-
- Smolensky MH, Hermida RC, Portaluppi F. Circadian mechanisms of 24‐hour blood pressure regulation and patterning. Sleep Med Rev. 2017;33:4–16. - PubMed
-
- Hassler C, Burnier M. Circadian variations in blood pressure: implications for chronotherapeutics. Am J Cardiovasc Drugs. 2005;5:7–15. - PubMed
-
- O'Brien E, Parati G, Stergiou G, Asmar R, Beilin L, Bilo G, Clement D, de la Sierra A, de Leeuw P, Dolan E, et al. European Society of Hypertension position paper on ambulatory blood pressure monitoring. J Hypertens. 2013;31:1731–1768. - PubMed
-
- Hermida RC, Crespo JJ, Otero A, Dominguez‐Sardina M, Moya A, Rios MT, Castineira MC, Callejas PA, Pousa L, Sineiro E, et al. Asleep blood pressure: significant prognostic marker of vascular risk and therapeutic target for prevention. Eur Heart J. 2018;39:4159–4171. - PubMed
-
- Birkenhager AM, van den Meiracker AH. Causes and consequences of a non‐dipping blood pressure profile. Neth J Med. 2007;65:127–131. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

