Patient reported outcome measures (PROMs) in sarcoidosis
- PMID: 32476819
- PMCID: PMC7170118
- DOI: 10.36141/svdld.v34i1.5760
Patient reported outcome measures (PROMs) in sarcoidosis
Abstract
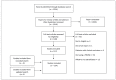
Patients with sarcoidosis present with a variety of symptoms which may impair many aspects of physical and mental well-being. Traditionally, clinicians have been concerned with physical health aspects of sarcoidosis, assessing disease activity and severity with radiological imaging, pulmonary function and blood tests. However, the most reported symptom of sarcoidosis patients, fatigue, has been shown not to correlate with the most commonly used parameters for monitoring disease activity. Studies have shown poor agreement between physicians and patients in assessing sarcoidosis symptoms. This underlines the importance of patient reported outcomes (PROs) in addition to traditional outcomes in order to provide a complete evaluation of the effects of interventions in clinical trials and everyday clinical assessment of sarcoidosis. We have undertaken a systematic review to identify and provide an overview of PRO concepts used in sarcoidosis assessment the past 20 years and to evaluate the tools used for measuring these concepts, called patient reported outcome measures (PROMs). Various PROMs have been used. By categorizing these PROMs according to outcome we identified the key PRO concepts for sarcoidosis to be Health Status and Quality of Life, Dyspnea, Fatigue, Depression, Anxiety and Stress and Miscellaneous. There is no perfect sarcoidosis-specific PROM to cover all concepts and future intervention studies should therefore contain multiple complementary questionnaires. Based on our findings we recommend the Fatigue Assessment Scale (FAS) for assessing fatigue. Dyspnea scores should be chosen based on their purpose; more research is needed to examine their validity in sarcoidosis. The Modified Medical Research Council Dyspnea Scale (MRC) can be used to screen for dyspnea and the Baseline Dyspnea Index (BDI) to detect changes in dyspnea. We recommend The World Health Organization Quality of Life assessment instrument (WHOQOL-100) for assessing quality of life, although a shorter questionnaire would be preferable. For assessing health status we recommend the Sarcoidosis Assessment Tool (SAT), and have great expectations for this new and promising assessment tool. Supplementary to the WASOG meeting of 2011's recommendation on assessing QoL, we recommend incorporating fatigue, dyspnea and HS assessment in clinical trials and everyday clinical assessment of sarcoidosis. (Sarcoidosis Vasc Diffuse Lung Dis 2017; 34: 2-17).
Keywords: PRO; PROM; clinical assessment; clinical trial; patient reported outcome; questionnaires; sarcoidosis.
Copyright: © 2017.
Similar articles
-
Predictors of cough-specific and generic quality of life in sarcoidosis patients.Sarcoidosis Vasc Diffuse Lung Dis. 2020;37(2):158-168. doi: 10.36141/svdld.v37i2.9234. Epub 2020 Jun 30. Sarcoidosis Vasc Diffuse Lung Dis. 2020. PMID: 33093779 Free PMC article.
-
Differences in symptom severity and health status impairment between patients with pulmonary and pulmonary plus extrapulmonary sarcoidosis.Respir Med. 2008 Nov;102(11):1636-42. doi: 10.1016/j.rmed.2008.05.001. Epub 2008 Aug 8. Respir Med. 2008. PMID: 18691860
-
Assessment of dyspnea in sarcoidosis using the Baseline Dyspnea Index (BDI) and the Transition Dyspnea Index (TDI).Respir Med. 2022 Jan;191:106436. doi: 10.1016/j.rmed.2021.106436. Epub 2021 May 4. Respir Med. 2022. PMID: 33992496
-
Assessing outcome measures used after rib fracture: A COSMIN systematic review.Injury. 2019 Nov;50(11):1816-1825. doi: 10.1016/j.injury.2019.07.002. Epub 2019 Jul 4. Injury. 2019. PMID: 31353094
-
Health-Related Quality of Life in Sarcoidosis.Semin Respir Crit Care Med. 2020 Oct;41(5):716-732. doi: 10.1055/s-0040-1710080. Epub 2020 Jun 24. Semin Respir Crit Care Med. 2020. PMID: 32583381 Review.
Cited by
-
Longitudinal validation of King's Sarcoidosis Questionnaire in a prospective cohort with mild sarcoidosis.ERJ Open Res. 2024 Nov 11;10(6):00160-2024. doi: 10.1183/23120541.00160-2024. eCollection 2024 Nov. ERJ Open Res. 2024. PMID: 39534770 Free PMC article.
-
Validity and Reliability of the Fatigue Severity Scale in a Real-World Interstitial Lung Disease Cohort.Am J Respir Crit Care Med. 2023 Jul 15;208(2):188-195. doi: 10.1164/rccm.202208-1504OC. Am J Respir Crit Care Med. 2023. PMID: 37099412 Free PMC article.
-
Scout - sarcoidosis outcomes taskforce. A systematic review of outcomes to inform the development of a core outcome set for pulmonary sarcoidosis.Sarcoidosis Vasc Diffuse Lung Dis. 2021;38(3):e2021034. doi: 10.36141/svdld.v38i3.10737. Epub 2021 Sep 30. Sarcoidosis Vasc Diffuse Lung Dis. 2021. PMID: 34744426 Free PMC article.
-
Patient-centered Outcomes Research in Interstitial Lung Disease: An Official American Thoracic Society Research Statement.Am J Respir Crit Care Med. 2021 Jul 15;204(2):e3-e23. doi: 10.1164/rccm.202105-1193ST. Am J Respir Crit Care Med. 2021. PMID: 34283696 Free PMC article.
-
Comprehensive Care for Patients with Sarcoidosis.J Clin Med. 2020 Feb 1;9(2):390. doi: 10.3390/jcm9020390. J Clin Med. 2020. PMID: 32024123 Free PMC article. Review.
References
-
- Valeyre D, Prasse A, Nunes H, Uzunhan Y, Brillet PY, Muller-Quernheim J. Sarcoidosis. Lancet. 2014 Mar 29;383(9923):1155–67. - PubMed
-
- De Vries J, Lower EE, Drent M. Quality of life in sarcoidosis: Assessment and management. Semin Respir Crit Care Med. 2010 Aug;31(4):485–93. - PubMed
-
- Drent M, Wirnsberger RM, De Vries J, Van Dieijen-Visser MP, Wouters EFM, Schols AMWJ. Association of fatigue with an acute phase response in sarcoidosis. Eur Respir J. 1999;13(4):718–22. - PubMed
-
- Cox CE, Donohue JF, Brown CD, Kataria YP, Judson MA. Health-related quality of life of persons with sarcoidosis. Chest. 2004;125(3):997–1004. - PubMed
-
- Judson MA, Mack M, Beaumont JL, Watt R, Barnathan ES, Victorson DE. Validation and important differences for the sarcoidosis assessment tool. A new patient-reported outcome measure. Am J Respir Crit Care Med. 2015 Apr 1;191(7):786–95. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous