Heparin as a therapy for COVID-19: current evidence and future possibilities
- PMID: 32519894
- PMCID: PMC7381711
- DOI: 10.1152/ajplung.00199.2020
Heparin as a therapy for COVID-19: current evidence and future possibilities
Abstract
Coronavirus disease 2019 (COVID-19), the clinical syndrome associated with infection by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), has impacted nearly every country in the world. Despite an unprecedented focus of scientific investigation, there is a paucity of evidence-based pharmacotherapies against this disease. Because of this lack of data-driven treatment strategies, broad variations in practice patterns have emerged. Observed hypercoagulability in patients with COVID-19 has created debate within the critical care community on the therapeutic utility of heparin. We seek to provide an overview of the data supporting the therapeutic use of heparin, both unfractionated and low molecular weight, as an anticoagulant for the treatment of SARS-CoV-2 infection. Additionally, we review preclinical evidence establishing biological plausibility for heparin and synthetic heparin-like drugs as therapies for COVID-19 through antiviral and anti-inflammatory effects. Finally, we discuss known adverse effects and theoretical off-target effects that may temper enthusiasm for the adoption of heparin as a therapy in COVID-19 without confirmatory prospective randomized controlled trials. Despite previous failures of anticoagulants in critical illness, plausibility of heparin for COVID-19 is sufficiently robust to justify urgent randomized controlled trials to determine the safety and effectiveness of this therapy.
Keywords: COVID-19; heparin; venous thromboembolism.
Conflict of interest statement
No conflicts of interest, financial or otherwise, are declared by the authors.
Figures
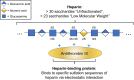


References
-
- Abraham E, Reinhart K, Opal S, Demeyer I, Doig C, Rodriguez AL, Beale R, Svoboda P, Laterre PF, Simon S, Light B, Spapen H, Stone J, Seibert A, Peckelsen C, De Deyne C, Postier R, Pettilä V, Sprung CL, Artigas A, Percell SR, Shu V, Zwingelstein C, Tobias J, Poole L, Stolzenbach JC, Creasey AA; OPTIMIST Trial Study Group . Efficacy and safety of tifacogin (recombinant tissue factor pathway inhibitor) in severe sepsis: a randomized controlled trial. JAMA 290: 238–247, 2003. doi:10.1001/jama.290.2.238. - DOI - PubMed
-
- Arnold K, Xu Y, Sparkenbaugh EM, Li M, Han X, Zhang X, Xia K, Piegore M, Zhang F, Zhang X, Henderson M, Pagadala V, Su G, Tan L, Park PW, Stravitz RT, Key NS, Linhardt RJ, Pawlinski R, Xu D, Liu J. Design of anti-inflammatory heparan sulfate to protect against acetaminophen-induced acute liver failure. Sci Transl Med 12: eaav8075, 2020. doi:10.1126/scitranslmed.aav8075. - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

