Long-term Safety of Oral Systemic Therapies for Psoriasis: A Comprehensive Review of the Literature
- PMID: 32529393
- PMCID: PMC7367959
- DOI: 10.1007/s13555-020-00409-4
Long-term Safety of Oral Systemic Therapies for Psoriasis: A Comprehensive Review of the Literature
Abstract
Oral systemic therapies are important treatment options for patients with moderate-to-severe psoriasis, either as monotherapy or in therapy-recalcitrant cases as combination therapy with phototherapy, other oral systemics or biologics. Long-term treatment is needed to maintain sufficient disease control in psoriasis, but continuous use of systemic treatments is limited by adverse events (AEs) and cumulative toxicity risks. The primary aim of this comprehensive literature review was to examine the long-term safety profiles of oral agents commonly used in the treatment of adults with psoriasis. Searches were conducted in EMBASE and PubMed up to November 2018, and 157 relevant publications were included. Long-term treatment with acitretin could be associated with skeletal toxicity and hepatotoxicity, although evidence for skeletal toxicity is mixed and hepatotoxicity is rare, particularly at low doses. Other safety issues include hyperlipidaemia and potential for teratogenicity up to 2-3 years after discontinuation of treatment. There is a paucity of data on long-term treatment with apremilast. Continued exposure to apremilast does not seem to increase the incidence of common AEs, such as gastrointestinal (GI) AEs, upper respiratory tract infections and headache, while the long-term risks for depression, suicidal thoughts and weight loss are unknown. Long-term ciclosporin treatment is associated with renal toxicity, hypertension, non-melanoma skin cancer, neurological AEs and GI AEs. Long-term methotrexate treatment is associated with hepatotoxicity, GI AEs, haematological toxicity, renal toxicity and alopecia. Finally, long-term treatment with fumaric acid esters (FAE) is associated with GI AEs, flushing, lymphocytopenia, proteinuria and elevated liver enzymes. Median drug survival estimates varied considerably: ~ 2.9-9.7 months for apremilast; ~ 5.4 months for ciclosporin; ~ 8.6 months for acitretin; ~ 12.1-21.6 months for methotrexate; and ~ 54.8 months for FAE. These long-term safety profiles may help to guide clinicians to select the optimal oral systemic treatment for the long-term treatment of psoriasis in adults.
Keywords: Adverse events; Drug survival; Long-term; Psoriasis; Safety; Systemic therapy.
Conflict of interest statement
Deepak M. W. Balak is a consultant/speaker for AbbVie, Almirall, Celgene, Eli Lilly, Janssen, LEO Pharma, Novartis and Sanofi Genzyme, and has received research grants from LEO Pharma. Sascha Gerdes has been an adviser for and/or received speakers’ honoraria and/or received grants from, and/or participated in clinical trials for Abbott/AbbVie, Affibody AB, Akari Therapeutics Plc, Almirall-Hermal, Amgen, Anaptys Bio, Baxalta, Bayer Health Care, Biogen Idec, Bioskin, Boehringer Ingelheim, Celgene, Centocor, Dermira, Eli Lilly, Foamix, Forward Pharma, Galderma, Hexal AG, Incyte Inc., Isotechnika, Janssen-Cilag, Johnson & Johnson, Kymab, LEO Pharma, Medac, Merck Serono, Mitsubishi Tanabe, Mölnlycke Health Care, MSD, Novartis, Pfizer, Polichem S.A., Principia Biopharma, Regeneron Pharmaceutical, Sandoz Biopharmaceuticals, Sanofi-Aventis, Schering-Plough, Sienna Biopharmaceuticals, Takeda, Teva, Trevi Therapeutics, UCB Pharma, VBL Therapeutics and Wyeth Pharma. Aurora Parodi has received speaker grants from and/or participated in clinical trials for AbbVie, Almirall, Celgene, Galderma, Jannsen-Cilag, LEO Pharma, Lily, Novartis, Pfizer and UCB. Laura Salgado-Boquete has received fees from AbbVie, Almirall, Celgene, Janssen, LEO Pharma, Lilly, Novartis, MSD and Pfizer.
Figures
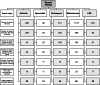
References
-
- Menter A, Korman NJ, Elmets CA, et al. Guidelines of care for the management of psoriasis and psoriatic arthritis: section 6. Guidelines of care for the treatment of psoriasis and psoriatic arthritis: case-based presentations and evidence-based conclusions. J Am Acad Dermatol. 2011;65(1):137–174. doi: 10.1016/j.jaad.2010.11.055. - DOI - PubMed
-
- Menter A, Korman NJ, Elmets CA, et al. Guidelines of care for the management of psoriasis and psoriatic arthritis: section 4. Guidelines of care for the management and treatment of psoriasis with traditional systemic agents. J Am Acad Dermatol. 2009;61(3):451–485. doi: 10.1016/j.jaad.2009.03.027. - DOI - PubMed
-
- Nakamura M, Koo J. Safety considerations with combination therapies for psoriasis. Expert Opin Drug Saf. 2020;19(4):489–98. - PubMed
-
- Armstrong AW, Bagel J, Van Voorhees AS, Robertson AD, Yamauchi PS. Combining biologic therapies with other systemic treatments in psoriasis: evidence-based, best-practice recommendations from the Medical Board of the National Psoriasis Foundation. JAMA Dermatol. 2015;151(4):432–438. doi: 10.1001/jamadermatol.2014.3456. - DOI - PubMed
Publication types
LinkOut - more resources
Full Text Sources

