Zim CHIC: A cohort study of immune changes in the female genital tract associated with initiation and use of contraceptives
- PMID: 32533883
- PMCID: PMC7507197
- DOI: 10.1111/aji.13287
Zim CHIC: A cohort study of immune changes in the female genital tract associated with initiation and use of contraceptives
Abstract
Problem: Contraceptive hormones are systemically active, potent, and likely to invoke biological responses other than known fertility regulation impacts. We hypothesized that initiation of depot medroxyprogesterone acetate (DMPA) would increase genital HIV-target-cells and soluble immune mediators compared with baseline and initiation of other contraceptive methods.
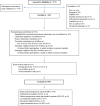
Method of study: We collected cervical cytobrushes and cervicovaginal fluid from healthy Zimbabwean women aged 18-34 to assess immune cell populations, cytokines, and innate anti-HIV activity at baseline and after 30, 90, and 180 days use of DMPA (n = 38), norethisterone enanthate (n = 41), medroxyprogesterone acetate/estradiol cypionate (n = 36), levonorgestrel implant (n = 43), etonogestrel implant (n = 47), or copper intrauterine device (Cu-IUD) (n = 45). Cells were quantified by flow cytometry, cytokines were detected by multiplex assays, and innate anti-HIV activity was assessed by in vitro HIV challenge.
Results: Compared to baseline, the number of cervical HIV target cells (#CD4 cells P < .04 and #CD11c cells P < .04), the concentration of the inflammatory cytokine IL-1β (P < .01), and the innate in vitro anti-HIV activity (P < .001) significantly decreased following DMPA initiation. In Cu-IUD users, genital HIV target cells increased (#CD4 cells P < .001, #CD4CCR5 cells P = .02, #CD4CD69 cells P < .001, #CD8CD69 P = .01, and #CD11c cells P = .003) at day 30 and resolved by day 180. IFN-γ (P < .001), IL-1β (P < .001), IL-6 (P < .001), IL-8 (P < .001), IL-10 (P < .01), and RANTES (P < .001) were also significantly increased at day 30. Minimal alterations were observed following initiation of subdermal implantable contraceptives.
Conclusions: This head-to-head study compared six contraceptives and found increased HIV target cells and cervical inflammation temporally associated with Cu-IUD initiation. Use of hormonal contraception, including DMPA, did not increase cervical HIV target cells or inflammation. Clinical Trial Number: NCT02038335.
Keywords: CCR5; biomarkers; contraception; copper; medroxyprogesterone acetate; receptors.
© 2020 The Authors. American Journal of Reproductive Immunology published by John Wiley & Sons Ltd.
Conflict of interest statement
The funder had no role in study design, data collection, data analysis, data interpretation, or manuscript writing. The corresponding author had full access to all study data and final responsibility for the decision to submit for publication. SLA has served as a consultant to Merck Sharp & Dohme Corp and has received research grants from Mithra and Evofem. SLH is a consultant for Merck, Pfizer, Lupin, Hologic, Pfizer, and Daré Bioscience, and receives research funding from Cepheid, Becton‐Dickinson, and Curatek. All other authors declare no competing interests.
Figures





References
-
- United Nations. Department of Economic and Social Affairs, Population Division . Trends in Contraceptive Use Worldwide 2015 (ST/ESA/SER.A/349). 2015.
-
- Birth Control Around the World: Mapping Methods of Contraception | Superdrug™ . https://onlinedoctor.superdrug.com/birth‐control‐around‐the‐world/. Accessed February 15, 2019
-
- Evidence for Contraceptive Options and HIV Outcomes (ECHO) Trial Consortium . HIV incidence among women using intramuscular depot medroxyprogesterone acetate, a copper intrauterine device, or a levonorgestrel implant for contraception: a randomised, multicentre, open‐label trial. Lancet. 2019;394(10195):303‐313. - PMC - PubMed
Publication types
MeSH terms
Substances
Associated data
LinkOut - more resources
Full Text Sources
Medical
Research Materials

