Involvement of cardiovascular system as the critical point in coronavirus disease 2019 (COVID-19) prognosis and recovery
- PMID: 32534109
- PMCID: PMC7286275
- DOI: 10.1016/j.hjc.2020.05.004
Involvement of cardiovascular system as the critical point in coronavirus disease 2019 (COVID-19) prognosis and recovery
Abstract
The novel coronavirus disease 2019 (COVID-19) pandemic has already caused more than 300,000 deaths worldwide. Several studies have elucidated the central role of cardiovascular complications in the disease course. Herein, we provide a concise review of current knowledge regarding the involvement of cardiovascular system in the pathogenesis and prognosis of COVID-19. We summarize data from 21 studies involving in total more than 21,000 patients from Asia, Europe, and the USA indicating that severe disease is associated with the presence of myocardial injury, heart failure, and arrhythmias. Additionally, we present the clinical and laboratory differences between recovered and deceased patients highlighting the importance of cardiac manifestations. For the infected patients, underlying cardiovascular comorbidities and particularly existing cardiovascular disease seem to predispose to the development of cardiovascular complications, which are in turn associated with higher mortality rates. We provide mechanistic insights into the underlying mechanisms including direct myocardial damage by the virus and the consequences of the hyperinflammatory syndrome developed later in the disease course. Finally, we summarize current knowledge on therapeutic modalities and recommendations by scientific societies and experts regarding the cardiovascular management of patients with COVID-19.
Keywords: COVID-19; Cardiovascular comorbidities; Cardiovascular complications; Pandemic; SARS-CoV-2.
Copyright © 2020 Hellenic Society of Cardiology. Published by Elsevier B.V. All rights reserved.
Figures

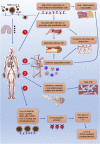



References
-
- World Health Organization Coronavirus disease (COVID-19) outbreak. https://www.who.int
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

