The Relationship between Post-colonoscopy Colorectal Cancer and Quality Indicators of Colonoscopy: The Latest Single-center Cohort Study with a Review of the Literature
- PMID: 32536675
- PMCID: PMC7364247
- DOI: 10.2169/internalmedicine.4212-19
The Relationship between Post-colonoscopy Colorectal Cancer and Quality Indicators of Colonoscopy: The Latest Single-center Cohort Study with a Review of the Literature
Abstract
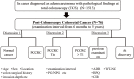
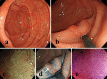
Objective This study aims to elucidate the association between the clinical characteristics of post-colonoscopy colorectal cancer (PCCRC) and quality indicators (QIs) of colonoscopy. Methods Patients with PCCRC who underwent total colonoscopy (TCS) and were histologically diagnosed with adenocarcinoma within six months to five years of the last examination were included in this study. PCCRC and normally detected cancer (NDC) identified within the same period were compared in terms of their clinicopathological characteristics. Furthermore, the QIs at PCCRC detection were compared to those at the last examination. Results Patients with PCCRC had a significantly higher rate of colon surgery history than those with NDC (PCCRC: 25/76, 32.9%; NDC: 31/1,437, 2.2%; p<0.001), but the invasion depth in these patients was significantly shallower (PCCRC: ≤Tis/≥T1, 37/39; NDC: ≤Tis/≥T1, 416/1,021; p<0.001). Among patients with PCCRC, the T1b group had significantly more non-polypoid growth (NPG)-type cases than PG-type CRC cases (p=0.018). The adenoma detection rate (ADR) of colonoscopists performing TCS was 30.2-52.8%. Furthermore, the ADR of colonoscopists at the time of PCCRC detection (36.7%±5.9%) was significantly higher than that of colonoscopists who performed the last examination (34.9%±4.4%; p=0.034). The withdrawal time for negative colonoscopy (WT-NC) at detection was significantly longer than that at the last examination (at detection: 494.3±253.8 s; at last examination: 579.5±243.6 s; p=0.010). Conclusion Given that these PCCRC cases were post-colon surgery cases, had a long WT-NC, and were detected by colonoscopists with a high ADR, most cases showed lesions that were missed during the previous colonoscopy. Caution should be practiced in order to avoid missing flat, NPG-type tumors.
Keywords: adenoma detection rate; interval cancer; polypoid growth; post-colonoscopy colorectal cancer; quality indicator.
Conflict of interest statement
Figures
References
-
- Brenner H, Chang-Claude J, Seiler CM, et al. Interval cancers after negative colonoscopy: population-based case-control study. Gut 61: 1576-1582, 2012. - PubMed
-
- Samadder NJ, Curtin K, Tuohy TM, et al. Characteristics of missed or interval colorectal cancer and patient survival: a population-based study. Gastroenterology 146: 950-960, 2014. - PubMed
-
- Lieberman DA, Rex DK, Winawer SJ, et al. Guidelines for colonoscopy surveillance after screening and polypectomy: a consensus update by the US Multi-Society Task Force on Colorectal Cancer. Gastroenterology 143: 844-857, 2012. - PubMed
-
- Singh S, Singh PP, Murad MH, et al. Prevalence, risk factors, and outcomes of interval colorectal cancers: a systematic review and meta-analysis. Am J Gastroenterol 109: 1375-1389, 2014. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials

