Intravenous versus topical tranexamic acid in lumbar interbody fusion: A protocol of randomized controlled trial
- PMID: 32541498
- PMCID: PMC7302681
- DOI: 10.1097/MD.0000000000020619
Intravenous versus topical tranexamic acid in lumbar interbody fusion: A protocol of randomized controlled trial
Expression of concern in
-
Expression of Concern: Study Protocols.Medicine (Baltimore). 2025 Nov 7;104(45):e46330. doi: 10.1097/MD.0000000000046330. Medicine (Baltimore). 2025. PMID: 41204616 Free PMC article. No abstract available.
Abstract
Background: Questions still remain about the safest and most effective route of administration for tranexamic acid (TXA) in lumbar interbody fusion. As such, the goal of this randomized clinical trial was to assess the efficacy and safety of topical TXA compared with intravenous TXA in lumbar interbody fusion.
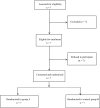
Methods: This was a prospectively randomized trial that investigated the effectiveness and safety of the intravenous and topical administrations of TXA with regard to lumbar interbody fusion. Approval from Clinical Studies Ethical Committee in our hospital was obtained. The patients were randomized to 1 of 2 treatment options:Patients, surgeons, anesthesiologists, nurses, and research assistants collecting data were blinded to group allocation. The primary outcome measures were perioperative calculated blood loss, total drain output at 24 hours, and perioperative blood transfusion rate. Secondary outcomes included an analysis of complications, namely symptomatic venous thromboembolism, cerebrovascular accident, and arterio-occlusive events. Data were analyzed using the statistical software package SPSS version 25.0 (Chicago, IL).
Results: There are several limitations to this study. We did not include a group of patients who did not receive TXA. Another potential limitation is that the study population contains heterogeneity such as varying patient diagnosis and surgical technique/approach. Despite these limitations, the validity of our results should be maintained, as the same methodology was applied to both treatment arms.
Trial registration: This study protocol was registered in Research Registry (researchregistry5564).
Conflict of interest statement
The authors have no conflicts of interest to disclose.
References
-
- Mu X, Wei J, Wang C, et al. Intravenous administration of tranexamic acid significantly reduces visible and hidden blood loss compared with its topical administration for double-segment posterior lumbar interbody fusion: a single-center, placebo-controlled, randomized trial. World Neurosurg 2019;122:e821–7. - PubMed
-
- Lopez-Balderas N, Bravo E, Camara M, et al. Seroprevalence of hepatitis viruses and risk factors in blood donors of Veracruz, Mexico. J Infect Dev Ctries 2015;9:274–82. - PubMed
-
- Risberg B. The response of the fibrinolytic system in trauma. Acta Chir Scand Suppl 1985;522:245–71. - PubMed
-
- Dunn CJ, Goa KL. Tranexamic acid: a review of its use in surgery and other indications. Drugs 1999;57:1005–32. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Research Materials