Alterations in the Gut Microbiome in the Progression of Cirrhosis to Hepatocellular Carcinoma
- PMID: 32546668
- PMCID: PMC7300357
- DOI: 10.1128/mSystems.00153-20
Alterations in the Gut Microbiome in the Progression of Cirrhosis to Hepatocellular Carcinoma
Abstract
Hepatocellular carcinoma (HCC) is the second leading cause of cancer-related mortality worldwide. While cirrhosis is the main risk factor for HCC, the factors influencing progression from cirrhosis to HCC remain largely unknown. Gut microbiota plays a key role in liver diseases; however, its association with HCC remains elusive. This study aimed to elucidate microbial differences between patients with HCC-associated cirrhosis (HCC-cirrhosis) and cirrhotic patients without HCC and healthy volunteers and to explore the associations between diet, lifestyle, and the microbiome of these patients. Fecal samples and food frequency questionnaires were collected from 95 individuals (30 HCC-cirrhosis patients, 38 cirrhotic patients without HCC, and 27 age- and body mass index [BMI]-matched healthy volunteers). 16S rRNA gene sequencing was performed. Bacterial richness in cirrhosis and HCC-cirrhosis patients was significantly lower than in healthy controls. The HCC-cirrhosis group was successfully classified with an area under the curve (AUC) value of 0.9 based on the dysbiotic fecal microbial signature. The HCC-cirrhosis group had a significant overrepresentation of Clostridium and CF231 and reduced Alphaproteobacteria abundance compared to cirrhotic patients without HCC. Patients with HCC-cirrhosis who were overweight displayed significantly decreased bacterial richness and altered microbiota composition compared to their normal-weight counterparts. There was a significant correlation in the HCC-cirrhosis group between intake of artificial sweeteners and the presence of Akkermansia muciniphila A unique microbial signature was observed in patients with HCC-cirrhosis, irrespective of cirrhosis stage, diet, or treatment. BMI, dietary sugar, and artificial sweeteners were significantly associated with alterations in the microbiome of HCC-cirrhosis patients. However, the increased abundance of Clostridium and CF231 observed in HCC-cirrhosis patients was not influenced by environmental factors, implying that this change was due to development of HCC.IMPORTANCE Development of hepatocellular carcinoma in patients with cirrhosis is associated with alterations in intestinal microbiota, including an escalation of dysbiosis and reduced bacterial richness. This study demonstrates that reduced bacterial richness and dysbiosis escalate with the progression of cirrhosis from compensated to decompensated cirrhosis and to HCC-associated cirrhosis (HCC-cirrhosis). Moreover, we report for the first time the effect of environmental factors on HCC-cirrhosis. Excess weight was associated with increased dysbiosis in patients with HCC compared to their normal-weight counterparts. Moreover, fatty liver, consumption of artificial sweeteners, and high-sugar foods were associated with altered microbial composition, including altered levels of Akkermansia muciniphila in HCC-cirrhosis. We have successfully determined that levels of Alphaproteobacteria and the two genera CF231 and Clostridium are significantly altered in cirrhotic patients who develop hepatocellular carcinoma, independently of cirrhosis severity and dietary habits.
Keywords: A. muciniphila; cirrhosis; diet; gut microbiome; hepatocellular carcinoma; microbiome.
Copyright © 2020 Lapidot et al.
Figures



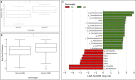

References
-
- World Health Organization. 2018. Cancer. World Health Organization, Geneva, Switzerland.
-
- Yoshimoto S, Loo TM, Atarashi K, Kanda H, Sato S, Oyadomari S, Iwakura Y, Oshima K, Morita H, Hattori M, Honda K, Ishikawa Y, Hara E, Ohtani N. 2013. Obesity-induced gut microbial metabolite promotes liver cancer through senescence secretome. Nature 499:97–101. doi:10.1038/nature12347. - DOI - PubMed
LinkOut - more resources
Full Text Sources

