Surgical Options for Aortic Root Replacement in Destructive Endocarditis
- PMID: 32549097
- PMCID: PMC7299601
- DOI: 10.21470/1678-9741-2020-0020
Surgical Options for Aortic Root Replacement in Destructive Endocarditis
Abstract
Objective: To analyze patients' preoperative characteristics, surgical data, postoperative courses, and short- and long-term outcomes after implantation of different full-root prostheses for destructive aortic valve endocarditis.
Methods: Between 1999 and 2018, 80 patients underwent aortic root replacement due to infective endocarditis in our institution. We analyzed the abovementioned data with standard statistical methods.
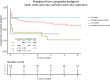
Results: The Freestyle stentless porcine prostheses were implanted in 53 (66.25%) patients, biological valve conduits in 13 (16.25%), aortic root homografts in nine (11.25%), and mechanical valve conduits in five (6.25%). There were no significant preoperative differences between the groups. The incidence of postoperative complications and intensive care unit length of stay did not differ significantly between the groups. The 30-day mortality rate was low among Freestyle patients (n=8, 15.1%) and high in the mechanical conduit cohort (n=3, 60%), though with borderline statistical significance (P=0.055). The best mean survival rates were observed after homograft (13.7 years) and stentless prosthesis (8.1 years) implantation, followed by biological (2.8 years) and mechanical (1.4 years) conduits (P=0.014). The incidence of reoperations was low in the mechanical conduit group (0) and stentless bioroot group (n=1, 1.9%), but two (15.4%) patients with biological conduits and three (33.3%) patients with homografts required reoperations in the investigated follow-up period (P=0.005).
Conclusion: In patients with the destructive form of aortic valve endocarditis, homografts and stentless porcine xenografts offer better survival rates than stented valve conduits; however, the reoperation rate among patients who received homograft valves is high.
Keywords: Allografts; Aortic Valve; Endocarditis, Bacterial; Heterografts; Reoperation; Stents; Transplantation, Heterologous.
Conflict of interest statement
No conflict of interest.
Figures
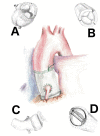

References
-
- Anantha Narayanan M, Mahfood Haddad T, Kalil AC, Kanmanthareddy A, Suri RM, Mansour G, et al. Early versus late surgical intervention or medical management for infective endocarditis: a systematic review and metaanalysis. Heart. 2016;102(12):950–957. doi: 10.1136/heartjnl-2015-308589. - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
