Stool cultures show a lack of impact in the management of acute gastroenteritis for hospitalized patients in the Bronx, New York
- PMID: 32582380
- PMCID: PMC7310251
- DOI: 10.1186/s13099-020-00369-2
Stool cultures show a lack of impact in the management of acute gastroenteritis for hospitalized patients in the Bronx, New York
Abstract
Background: Acute gastroenteritis (AGE) is diagnosed with a presentation of > 1 episode of vomiting and > 3 episodes of diarrhea in a 24-h period. Treatment is supportive, however, in severe cases antibacterial treatment may be indicated. Stool cultures can detect the responsible pathogenic bacteria and can guide antibiotic treatment, however, the indication for and efficacy of stool cultures is debatable. This study aimed to address the clinical utility of stool cultures in patients diagnosed with AGE.
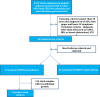
Methods: A retrospective, multicenter study was performed in patients admitted for AGE from 2012 to 2014. Patient charts were obtained through hospital software using ICD-9 codes for AGE. Inclusion criteria was a documented diagnosis of AGE, age of 18 years or older, symptoms of both upper GI symptoms of abdominal pain and/or nausea and lower GI symptoms of diarrhea. Patients were classified into two main groups, those in whom (1) stool culture was obtained and (2) those in whom stool culture was not performed. Clinical features and outcomes were compared between groups. The diagnostic yield of stool cultures was assessed. All analysis were conducted using the Statistical Package for Social Science (SPSS).
Results: Of 2479 patient charts reviewed, 342 met the above criteria for AGE. 119 patients (34.8%) had stool cultures collected and 223 (65.2%) did not. Demographics, clinical features and serologic lab values are shown in Table 1. Of the 119 stool cultures performed, only 4% (n = 5) yielded growth of pathogenic bacteria (2 Pseudomonas spp, 2 Campylobacter spp, 1 Salmonella spp). The group who underwent stool culture had a higher percentage of patients with fevers (26% vs 13%,p < 0.003) and longer hospital length of stay (3.15 vs 2.28 days, p < 0.001) compared to the group that did not undergo stool cultures.
Conclusion: Stool cultures are commonly ordered when AGE is suspected. In our cohort, stool culture had a very low yield of detecting an underlying pathogen. Although patients who had stool cultures obtained were more likely to be febrile and to have a longer length of hospital stay than were those who did not have stool cultures, for the vast majority of patients, stool culture played little to no role in patient management. Further studies are needed to which patients benefit most from undergoing stool culture.
Keywords: Acute Diarrhea; Acute Gastroenteritis; Stool Cultures.
© The Author(s) 2020.
Conflict of interest statement
Competing interestsThe authors declare that they have no competing interests.
References
-
- Haines C, Sears C. Infectious enteritis and proctocolits. In: Sleisenger and Fordtran's gastrointestinal and liver disease. 10th ed. Philadelphia, PA: Elsevier; 2016. pp. 1896–929
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous