Bacterial and host determinants of cough aerosol culture positivity in patients with drug-resistant versus drug-susceptible tuberculosis
- PMID: 32601338
- PMCID: PMC8353872
- DOI: 10.1038/s41591-020-0940-2
Bacterial and host determinants of cough aerosol culture positivity in patients with drug-resistant versus drug-susceptible tuberculosis
Abstract
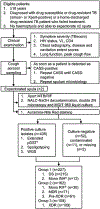
A burgeoning epidemic of drug-resistant tuberculosis (TB) threatens to derail global control efforts. Although the mechanisms remain poorly clarified, drug-resistant strains are widely believed to be less infectious than drug-susceptible strains. Consequently, we hypothesized that lower proportions of patients with drug-resistant TB would have culturable Mycobacterium tuberculosis from respirable, cough-generated aerosols compared to patients with drug-susceptible TB, and that multiple factors, including mycobacterial genomic variation, would predict culturable cough aerosol production. We enumerated the colony forming units in aerosols (≤10 µm) from 452 patients with TB (227 with drug resistance), compared clinical characteristics, and performed mycobacterial whole-genome sequencing, dormancy phenotyping and drug-susceptibility analyses on M. tuberculosis from sputum. After considering treatment duration, we found that almost half of the patients with drug-resistant TB were cough aerosol culture-positive. Surprisingly, neither mycobacterial genomic variants, lineage, nor dormancy status predicted cough aerosol culture positivity. However, mycobacterial sputum bacillary load and clinical characteristics, including a lower symptom score and stronger cough, were strongly predictive, thereby supporting targeted transmission-limiting interventions. Effective treatment largely abrogated cough aerosol culture positivity; however, this was not always rapid. These data question current paradigms, inform public health strategies and suggest the need to redirect TB transmission-associated research efforts toward host-pathogen interactions.
Figures






References
-
- Dheda K et al.The epidemiology, pathogenesis, transmission, diagnosis, and management of multidrug-resistant, extensively drug-resistant, and incurable tuberculosis. The lancet Respiratory medicine 5, 291–360 (2017). - PubMed
-
- Riley R et al.Infectiousness of air from a tuberculosis ward. Ultraviolet irradiation of infected air: comparative infectiousness of different patients. The American review of respiratory disease 85, 511 (1962). - PubMed
-
- Sultan L et al.Tuberculosis disseminators. A study of the variability of aerial infectivity of tuberculous patients. American Review of Respiratory Disease 82, 358–369 (1960). - PubMed
References for Methods
-
- Dheda K, Limberis JD, Pietersen E, et al.Outcomes, infectiousness, and transmission dynamics of patients with extensively drug-resistant tuberculosis and home-discharged patients with programmatically incurable tuberculosis: a prospective cohort study. The lancet Respiratory medicine 2017; 5(4): 269–81. - PubMed
-
- Wejse C, Gustafson P, Nielsen J, et al.TBscore: Signs and symptoms from tuberculosis patients in a low-resource setting have predictive value and may be used to assess clinical course. Scandinavian Journal of Infectious Diseases 2008; 40(2): 111–20. - PubMed
-
- te Riele JB, Buser V, Calligaro G, et al.Relationship between chest radiographic characteristics, sputum bacterial load, and treatment outcomes in patients with extensively drug-resistant tuberculosis. International Journal of Infectious Diseases. - PubMed
-
- World Health Organization. Mycobacteriology Laboratory Manual. 1st ed. Global Laboratory Initiative. Geneva, Switzerland; 2014.
-
- Rieder HL, Chonde TM, Myking H, et al.The public health service national tuberculosis reference laboratory and the national laboratory network; minimum requirements, role and operation in a low-income country: International Union Against Tuberculosis And Lung Disease (IUATLD); 1998.

