Erythromycin inhibits neutrophilic inflammation and mucosal disease by upregulating DEL-1
- PMID: 32603314
- PMCID: PMC7455085
- DOI: 10.1172/jci.insight.136706
Erythromycin inhibits neutrophilic inflammation and mucosal disease by upregulating DEL-1
Abstract
Macrolide antibiotics exert antiinflammatory effects; however, little is known regarding their immunomodulatory mechanisms. In this study, using 2 distinct mouse models of mucosal inflammatory disease (LPS-induced acute lung injury and ligature-induced periodontitis), we demonstrated that the antiinflammatory action of erythromycin (ERM) is mediated through upregulation of the secreted homeostatic protein developmental endothelial locus-1 (DEL-1). Consistent with the anti-neutrophil recruitment action of endothelial cell-derived DEL-1, ERM inhibited neutrophil infiltration in the lungs and the periodontium in a DEL-1-dependent manner. Whereas ERM (but not other antibiotics, such as josamycin and penicillin) protected against lethal pulmonary inflammation and inflammatory periodontal bone loss, these protective effects of ERM were abolished in Del1-deficient mice. By interacting with the growth hormone secretagogue receptor and activating JAK2 in human lung microvascular endothelial cells, ERM induced DEL-1 transcription that was mediated by MAPK p38 and was CCAAT/enhancer binding protein-β dependent. Moreover, ERM reversed IL-17-induced inhibition of DEL-1 transcription, in a manner that was dependent not only on JAK2 but also on PI3K/AKT signaling. Because DEL-1 levels are severely reduced in inflammatory conditions and with aging, the ability of ERM to upregulate DEL-1 may lead to a novel approach for the treatment of inflammatory and aging-related diseases.
Keywords: Immunology; Inflammation; Mouse models; Neutrophils; endothelial cells.
Conflict of interest statement
Figures



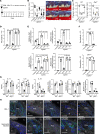


Similar articles
-
Antagonistic effects of IL-17 and D-resolvins on endothelial Del-1 expression through a GSK-3β-C/EBPβ pathway.Nat Commun. 2015 Sep 16;6:8272. doi: 10.1038/ncomms9272. Nat Commun. 2015. PMID: 26374165 Free PMC article.
-
The leukocyte integrin antagonist Del-1 inhibits IL-17-mediated inflammatory bone loss.Nat Immunol. 2012 Mar 25;13(5):465-73. doi: 10.1038/ni.2260. Nat Immunol. 2012. PMID: 22447028 Free PMC article.
-
Effects of Erythromycin on Osteoclasts and Bone Resorption via DEL-1 Induction in Mice.Antibiotics (Basel). 2021 Mar 17;10(3):312. doi: 10.3390/antibiotics10030312. Antibiotics (Basel). 2021. PMID: 33803007 Free PMC article.
-
Novel inflammatory pathways in periodontitis.Adv Dent Res. 2014 May;26(1):23-9. doi: 10.1177/0022034514526240. Adv Dent Res. 2014. PMID: 24736701 Free PMC article. Review.
-
Immune and regulatory functions of neutrophils in inflammatory bone loss.Semin Immunol. 2016 Apr;28(2):146-58. doi: 10.1016/j.smim.2016.02.002. Epub 2016 Feb 28. Semin Immunol. 2016. PMID: 26936034 Free PMC article. Review.
Cited by
-
Neutrophil elastase aggravates periodontitis by disrupting gingival epithelial barrier via cleaving cell adhesion molecules.Sci Rep. 2022 May 17;12(1):8159. doi: 10.1038/s41598-022-12358-3. Sci Rep. 2022. PMID: 35581391 Free PMC article.
-
Erythromycin Restores Osteoblast Differentiation and Osteogenesis Suppressed by Porphyromonas gingivalis Lipopolysaccharide.Pharmaceuticals (Basel). 2023 Feb 15;16(2):303. doi: 10.3390/ph16020303. Pharmaceuticals (Basel). 2023. PMID: 37259446 Free PMC article.
-
Pharmacokinetic/pharmacodynamic evaluation of gamithromycin against rabbit pasteurellosis.BMC Vet Res. 2024 Apr 20;20(1):147. doi: 10.1186/s12917-024-03988-y. BMC Vet Res. 2024. PMID: 38643185 Free PMC article.
-
Effects of Antibiotics upon the Gut Microbiome: A Review of the Literature.Biomedicines. 2020 Nov 16;8(11):502. doi: 10.3390/biomedicines8110502. Biomedicines. 2020. PMID: 33207631 Free PMC article. Review.
-
Effects of erythromycin dosage on clinical outcomes in stable non-cystic fibrosis bronchiectasis: A randomized controlled trial.Medicine (Baltimore). 2025 Jul 18;104(29):e43414. doi: 10.1097/MD.0000000000043414. Medicine (Baltimore). 2025. PMID: 40696686 Free PMC article. Clinical Trial.
References
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

