A Surviving Case of Acanthamoeba Granulomatous Amebic Encephalitis in a Hematopoietic Stem Cell Transplant Recipient
- PMID: 32603318
- PMCID: PMC7347033
- DOI: 10.12659/AJCR.923219
A Surviving Case of Acanthamoeba Granulomatous Amebic Encephalitis in a Hematopoietic Stem Cell Transplant Recipient
Abstract
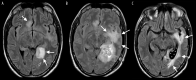
BACKGROUND Acanthamoeba are free-living amoebae with potential to infect immunocompromised hosts. The mortality rate of granulomatous amebic encephalitis (GAE) due to Acanthamoeba exceeds 90% and there are currently no reports of survival of this infection in recipients of hematopoietic stem cell transplant. CASE REPORT We report herein the case of a 32-year-old man presenting to our service with abrupt neurological deterioration and seizures 5 months after allogeneic stem cell transplantation for Hodgkin lymphoma. Clinical and imaging findings were non-specific at presentation. Multiple circumscribed, heterogenous, mass-like lesions were identified on MRI. Brain biopsy was performed and revealed multiple cysts and trophozoites suggesting a diagnosis of granulomatous amebic encephalitis. PCR testing confirmed Acanthamoeba. Treatment with miltefosine, metronidazole, azithromycin, fluconazole, pentamidine isethionate, and co-trimoxazole was instituted and the patient survived and shows continued improvement with intensive rehabilitation. CONCLUSIONS We report the first successful outcome in this setting. The diagnosis would have been missed on cerebrospinal fluid analysis alone, but was rapidly made by histological analysis of brain biopsy. This diagnostically challenging infection is likely under-recognized. Early brain biopsy and commencement of a prolonged miltefosine-containing anti-ameba regimen can be curative.
Conflict of interest statement
None.
Figures

References
-
- Schuster FL, Visvesvara GS. Opportunistic amoebae: Challenges in prophylaxis and treatment. Drug Resist Updat. 2004;7(1):41–51. - PubMed
-
- Anderlini P, Przepiorka D, Luna M, et al. Acanthamoeba meningoencephalitis after bone marrow transplantation. Bone Marrow Transplant. 1994;14(3):459–61. - PubMed
-
- Feingold JM, Abraham J, Bilgrami S, et al. Acanthamoeba meningoencephalitis following autologous peripheral stem cell transplantation. Bone Marrow Transplant. 1998;22(3):297–300. - PubMed
-
- Castellano-Sanchez A, Popp AC, Nolte FS, et al. Acanthamoeba castellani encephalitis following partially mismatched related donor peripheral stem cell transplantation. Transpl Infect Dis. 2003;5(4):191–94. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources

