Effect of Nebulized Verapamil on Oxygenation in Chronic Obstructive Pulmonary Disease (COPD) Patients Admitted to the Intensive Care Unit
- PMID: 32607114
- PMCID: PMC7309890
Effect of Nebulized Verapamil on Oxygenation in Chronic Obstructive Pulmonary Disease (COPD) Patients Admitted to the Intensive Care Unit
Abstract
Background: Many pharmacological and behavioral therapies have been investigated to improve oxygenation in the intensive care unit (ICU). In patients with chronic obstructive pulmonary disease (COPD), the purpose of therapy is to correct the ventilation perfusion (V/Q) mismatch. Agents, such as calcium blockers, can affect both ventilation and vasculature. The inhalation route allows a more rapid achievement of therapeutic effects with few systemic side effects. Therefore, the present study aimed to investigate the effect of nebulized verapamil on oxygenation in COPD patients.
Materials and methods: In this double-blind, randomized clinical trial, twenty hypoxic COPD patients, admitted to ICU, were treated with 10 mg of verapamil twice daily for three days. Also, twenty patients with COPD, who were matched in terms of age, sex, and severity of the disease, were enrolled in the control group and received nebulized normal saline. The oxygenation parameters were compared using an arterial blood gas (ABG) test before and after the intervention.
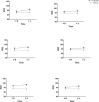
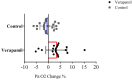
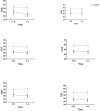
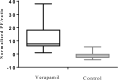
Results: The mean oxygen saturation was 91.2%±12.15 before verapamil inhalation, which increased to 95.75%±14.57 after receiving nebulized verapamil (P<0.05). Also, correction of blood pH, blood oxygen pressure, and oxygen ratio (PaO2/FIO2) were higher in patients receiving verapamil, compared to the control group. The length of hospital stay was similar in the two groups. During the first three days, 30% of patients in the verapamil group and 20% of patients in the control group were intubated.
Conclusion: Our results indicated that verapamil inhalation increased oxygen saturation and accelerated extubation in patients with COPD.
Keywords: Calcium Channel Blockers; Chronic Obstructive Pulmonary Disease; Oxygenation; Verapamil.
Copyright© 2019 National Research Institute of Tuberculosis and Lung Disease.
Figures
Similar articles
-
Clinical evaluation of nebulized verapamil in out-patients with pulmonary hypertension secondary to chronic obstructive pulmonary disease.Clin Respir J. 2022 Dec;16(12):802-811. doi: 10.1111/crj.13551. Epub 2022 Nov 6. Clin Respir J. 2022. PMID: 36336743 Free PMC article. Clinical Trial.
-
Therapeutic effects of nebulized verapamil on chronic obstructive pulmonary disease: A randomized and double-blind clinical trial.Clin Respir J. 2020 Apr;14(4):370-381. doi: 10.1111/crj.13142. Epub 2020 Jan 20. Clin Respir J. 2020. PMID: 31900997 Clinical Trial.
-
Severity of acidosis affects long-term survival in COPD patients with hypoxemia after intensive care unit discharge.Int J Chron Obstruct Pulmon Dis. 2018 May 9;13:1495-1506. doi: 10.2147/COPD.S159504. eCollection 2018. Int J Chron Obstruct Pulmon Dis. 2018. PMID: 29780244 Free PMC article.
-
Hemodynamic and gas exchange responses to inhalation of nitric oxide in patients with the acute respiratory distress syndrome and in hypoxemic patients with chronic obstructive pulmonary disease.Intensive Care Med. 1997 Jan;23(1):51-7. doi: 10.1007/s001340050290. Intensive Care Med. 1997. PMID: 9037640
-
Comparative efficacies of nebulized budesonide and systemic corticosteroids in the treatment of exacerbations of chronic obstructive pulmonary disease: A systematic review and meta-analysis.J Clin Pharm Ther. 2020 Jun;45(3):419-429. doi: 10.1111/jcpt.13095. Epub 2020 Jan 18. J Clin Pharm Ther. 2020. PMID: 31954070
Cited by
-
Cardiovascular diseases or type 2 diabetes mellitus and chronic airway diseases: mutual pharmacological interferences.Ther Adv Chronic Dis. 2023 May 31;14:20406223231171556. doi: 10.1177/20406223231171556. eCollection 2023. Ther Adv Chronic Dis. 2023. PMID: 37284143 Free PMC article. Review.
References
-
- Arokiasamy P, Uttamacharya, Kowal P, Capistrant BD, Gildner TE, Thiele E, et al. Chronic Noncommunicable Diseases in 6 Low- and Middle-Income Countries: Findings From Wave 1 of the World Health Organization’s Study on Global Ageing and Adult Health (SAGE). Am J Epidemiol 2017;185(6):414–428. - PMC - PubMed
-
- Varmaghani M, Farzadfar F, Sharifi F, Rashidian A, Moin M, Moradi-Lakeh M, et al. Prevalence of Asthma, COPD, and Chronic Bronchitis in Iran: A Systematic Review and Meta-analysis. Iran J Allergy Asthma Immunol 2016;15(2):93–104. - PubMed
LinkOut - more resources
Full Text Sources
