Evaluation of Urinary Neutrophil Gelatinase Associated Lipocalin and Kidney Injury Molecule-1 as Diagnostic Markers for Early Nephropathy in Patients with Type 2 Diabetes Mellitus
- PMID: 32612375
- PMCID: PMC7322140
- DOI: 10.2147/DMSO.S258678
Evaluation of Urinary Neutrophil Gelatinase Associated Lipocalin and Kidney Injury Molecule-1 as Diagnostic Markers for Early Nephropathy in Patients with Type 2 Diabetes Mellitus
Abstract
Purpose: The purpose of this study was evaluating the early diagnostic value of two specific tubular markers neutrophil gelatinase-associated lipocalin (NGAL) and kidney injury molecule-1 (KIM-1) in diabetes nephropathy.
Patients and methods: Cross-sectional study was carried in three groups of patients from 10/2017 to 10/2018 in Military Hospital 103. Group I included 30 healthy peoples with estimated glomerular filtration rate (eGFR) >60 mL/min/1.73 m2 and urine albumin creatinine ratio (uACR) <30 mg/g. Group II included 30 type 2 diabetic patients having uACR <30 mg/g, eGFR >60 mL/min/1.73 m2. Group III included 30 type 2 diabetic patients having uACR >30 mg/g, eGFR >60 mL/min/1.73 m2.
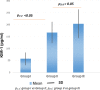
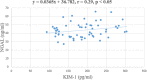
Results: Urine KIM-1 and NGAL increased progressively from control group (57.29 ± 25.91 pg/mL; 25.71 ± 13.69 ng/mL) to the group of diabetic patients with uACR <30 mg/g (167.06 ± 44.01 pg/mL; 37.42 ± 10.89 ng/mL) and the group of diabetic patients with uACR ≥30 mg/g) (p < 0.05). There were moderate correlations between KIM-1 (r = 0.48, p < 0.05) and NGAL (r = 0.45, p < 0.05) with uACR. There was a mild correlation between KIM-1 and NGAL (r = 0.29, p < 0.05). KIM-1 and NGAL are the independent tests to detect diabetic nephropathy. The sensivity and specificity of KIM-1 with cut-off value of 174.95 pg/mL were 62.37% and 73.48%, respectively; the sensivity and specificity of NGAL with cut-off value of 35.2 ng/mL were 60.45% and 70.37%, respectively.
Conclusion: KIM-1 and NGAL in urine are independent markers for early diagnostic diabetic nephropathy.
Keywords: albumin urine; diabetic kidney disease; urine albumin creatinin ratio.
© 2020 Quang et al.
Conflict of interest statement
The authors report no conflicts of interest in this work.
Figures


References
-
- Saeedi P, Petersohn I, Salpea P, et al. Global and regional diabetes prevalence estimates for 2019 and projections for 2030 and 2045: results from the international diabetes federation diabetes Atlas, 9th edition. Elsevier BV. 2019;57:1–10. - PubMed
-
- Harding JL, Pavkov ME, Magliano DJ, Shaw JE, Gregg EW. Global trends in diabetes complications: a review of current evidence. Diabetologia. 2019;62(1):3–16. - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

