Multiple milia formation in blistering diseases
- PMID: 32637544
- PMCID: PMC7330451
- DOI: 10.1016/j.ijwd.2020.03.045
Multiple milia formation in blistering diseases
Erratum in
-
Erratum regarding previously published articles.Int J Womens Dermatol. 2021 Sep 28;7(5Part B):867. doi: 10.1016/j.ijwd.2021.09.013. eCollection 2021 Dec. Int J Womens Dermatol. 2021. PMID: 35028405 Free PMC article.
Abstract
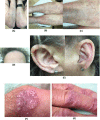
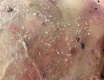
Background: Milia are superficial keratinous cysts seen as pearly white, dome-shaped lesions 1-2 mm in diameter. Milia are associated with diseases that cause subepidermal blistering, such as hereditary forms of epidermolysis bullosa, epidermolysis bullosa acquisita, bullous pemphigoid, bullous lichen planus, and porphyria cutanea tarda. Multiple eruptive milia are rare and more extensive in number than primary milia.
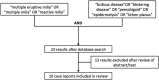
Objective: The aim of this study was to search the literature for cases of blistering diseases with multiple milia formation, especially in areas of the skin where there was no evidence of blistering or trauma, and review the interpretations of their pathogenesis.
Methods: We performed a literature search with the terms multiple milia and bullous diseases, pemphigoid, and pemphigus.
Results: Very few studies have investigated the origin of milia. Primary milia are thought to originate from the sebaceous collar of vellus hairs, and secondary milia are believed to derive from eccrine ducts more commonly than from overlying epidermis, hair follicles, or sebaceous ducts. Milia secondary to blisters or trauma are speculated to be produced through the regeneration process of disrupted sweat glands or hair follicles. Immunological predisposition, aberrant interaction between the hemidesmosomes, and the extracellular matrix components beneath the hemidesmosomes have been described with regard to the formation of numerous milia during recovery. Multiple milia could be a primary manifestation of dystrophic epidermolysis bullosa in skin areas without evidence of blistering.
Conclusion: The exact etiology of multiple milia remains unknown. Immunological predisposition and improper interaction between hemidesmosomes and extracellular matrix components are speculated to play a role in the formation of milia during recovery of bullous lesions in blistering diseases. Still, further studies on the triggering mechanisms of keratinocyte dysfunction in cases of multiple milia formation without evidence of prior blistering are needed.
Keywords: Autoimmune blistering diseases; Blistering diseases; Milia; Pemphigoid; Pemphigus.
© 2020 Published by Elsevier Inc. on behalf of Women's Dermatologic Society.
Figures
References
-
- Akaksa E., Nakano H., Takagi Y., Toyomaki Y., Sawamura D. Multiple milia as an isolated skin manifestation of dominant dystrophic epidermolysis bullosa: Evidence of phenotypic variability. Pediatr Dermatol. 2017;34(2):106–108. - PubMed
-
- Banfield C., Wojnarowska F., Allen J., George S., Venning V., Welsh K. The association of HLA-DQ7 with bullous pemphigoid is restricted to men. Br J Dermatol. 1998;138(6):1085–1090. - PubMed
-
- Berk D.R., Bayliss S.J. Milia: A review and classification. J Am Dermatol. 2008;59(6):1050–1063. - PubMed
Publication types
LinkOut - more resources
Full Text Sources