Factors associated with COVID-19-related death using OpenSAFELY
- PMID: 32640463
- PMCID: PMC7611074
- DOI: 10.1038/s41586-020-2521-4
Factors associated with COVID-19-related death using OpenSAFELY
Abstract
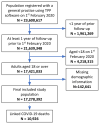
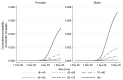
Coronavirus disease 2019 (COVID-19) has rapidly affected mortality worldwide1. There is unprecedented urgency to understand who is most at risk of severe outcomes, and this requires new approaches for the timely analysis of large datasets. Working on behalf of NHS England, we created OpenSAFELY-a secure health analytics platform that covers 40% of all patients in England and holds patient data within the existing data centre of a major vendor of primary care electronic health records. Here we used OpenSAFELY to examine factors associated with COVID-19-related death. Primary care records of 17,278,392 adults were pseudonymously linked to 10,926 COVID-19-related deaths. COVID-19-related death was associated with: being male (hazard ratio (HR) 1.59 (95% confidence interval 1.53-1.65)); greater age and deprivation (both with a strong gradient); diabetes; severe asthma; and various other medical conditions. Compared with people of white ethnicity, Black and South Asian people were at higher risk, even after adjustment for other factors (HR 1.48 (1.29-1.69) and 1.45 (1.32-1.58), respectively). We have quantified a range of clinical factors associated with COVID-19-related death in one of the largest cohort studies on this topic so far. More patient records are rapidly being added to OpenSAFELY, we will update and extend our results regularly.
Conflict of interest statement
All authors have completed the ICMJE uniform disclosure form at www.icmje.org/coi_disclosure.pdf and declare the following: CB JP FH JC SH are employees of TPP. AM was interim Chief Medical Officer NHS Digital April-Sept 2019 (left NHS Digital end Jan 2020) and Digital Clinical Champion NHS England 2014-2015. All other authors have no competing interests.
Figures



Comment in
-
Treating asthma in the COVID-19 pandemic.Thorax. 2020 Oct;75(10):822-823. doi: 10.1136/thoraxjnl-2020-215118. Epub 2020 Jun 10. Thorax. 2020. PMID: 32522762 No abstract available.
-
The Quest for Timely Insights into COVID-19 Should not Come at the Cost of Scientific Rigor.Epidemiology. 2021 Jan;32(1):e2. doi: 10.1097/EDE.0000000000001258. Epidemiology. 2021. PMID: 33065609 No abstract available.
-
Comment on Williamson et al. (OpenSAFELY): The Table 2 Fallacy in a Study of COVID-19 Mortality Risk Factors.Epidemiology. 2021 Jan;32(1):e1-e2. doi: 10.1097/EDE.0000000000001259. Epidemiology. 2021. PMID: 33065610 No abstract available.
-
The Authors Respond.Epidemiology. 2021 Jan;32(1):e2-e3. doi: 10.1097/EDE.0000000000001260. Epidemiology. 2021. PMID: 33105269 No abstract available.
-
COVID-19 and ethnicity: has history repeated itself?Thorax. 2021 Jun;76(6):537-538. doi: 10.1136/thoraxjnl-2021-216992. Epub 2021 Apr 9. Thorax. 2021. PMID: 33837142 No abstract available.
References
-
- COVID-19 situation reports. https://www.who.int/emergencies/diseases/novel-coronavirus-2019/situatio....
-
- WHO. WHO Director-General’s opening remarks at the media briefing on COVID-19 - 11 March 2020. 2020 https://web.archive.org/web/20200502133342/https://www.who.int/dg/speech....
-
- UK Government. Number of coronavirus (COVID-19) cases and risk in the UK. 2020 https://web.archive.org/web/20200501084711/https://www.gov.uk/guidance/c....
-
- NHS England. COVID-19 Daily Deaths. 2020 https://web.archive.org/web/20200501094237/https://www.england.nhs.uk/st...
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

