Influence of cement-augmented pedicle screws with different volumes of polymethylmethacrylate in osteoporotic lumbar vertebrae over the adjacent segments: a 3D finite element analysis
- PMID: 32660462
- PMCID: PMC7359596
- DOI: 10.1186/s12891-020-03498-6
Influence of cement-augmented pedicle screws with different volumes of polymethylmethacrylate in osteoporotic lumbar vertebrae over the adjacent segments: a 3D finite element analysis
Abstract
Background: Polymethylmethacrylate (PMMA) is commonly used for cement-augmented pedicle screw instrumentation (CAPSI) to improve the fixation stability and reduce the risk of screw loosening in the osteoporotic thoracolumbar spine. Biomechanical researches have shown that various dose of cement (1-3 ml) can be injected to enhance screw stability. To date, there have been no studies on the relationship between adjacent segment degeneration and the volume of PMMA. This study aimed to explore the influence of CAPSI with different volumes of PMMA in osteoporotic lumbar vertebrae over adjacent segments by using finite element analysis.
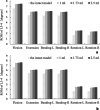
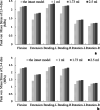
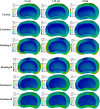
Methods: Seven different finite element models were reconstructed and simulated under different loading conditions, including (1) an intact model, (2) three single-level CAPSI models with different volumes of PMMA (1, 1.73, and 2.5 ml), and (3) three double-level CAPSI models with different volumes of PMMA (1, 1.73, and 2.5 ml). To improve the accuracy of the finite element analysis, the models of the injectable pedicle screw and bone cement were created by using a three-dimensional scanning machine and the CAPSI patient's CT data, respectively. The range of motion (ROM), the stress of intervertebral discs, and the stress of facet in the adjacent segment were comparatively analyzed among the different models.
Results: The ROMs of the different segments were compared with experimental data, with good agreement under the different load conditions (21.3°, 13.55°, 13.99°, and 6.11° in flexion, extension, bending, and rotation at L3-S1 level, respectively). Compared with the intact model, the ROM, disc stresses, and facet stress in adjacent segments were found to be higher in the six operative models. Otherwise, with a larger volume of PMMA injected, the ROM, disc stresses, and facet stress slightly increased at the adjacent segment. However, the differences were insignificant with the biggest difference less than 3.8%.
Conclusions: CAPSI could increase the incidence of disk degeneration in the adjacent segment, while within a certain range, different volumes of PMMA provided an approximate impact over the adjacent segment degeneration.
Keywords: Adjacent segment degeneration; Cement-augmented pedicle screws; Finite element analysis; Polymethylmethacrylate.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures




Similar articles
-
Influence of cement-augmented pedicle screw instrumentation in an osteoporotic lumbosacral spine over the adjacent segments: a 3D finite element study.J Orthop Surg Res. 2020 Apr 7;15(1):132. doi: 10.1186/s13018-020-01650-5. J Orthop Surg Res. 2020. PMID: 32264901 Free PMC article.
-
Biomechanical comparative study of the stability of injectable pedicle screws with different lateral holes augmented with different volumes of polymethylmethacrylate in osteoporotic lumbar vertebrae.Spine J. 2018 Sep;18(9):1637-1644. doi: 10.1016/j.spinee.2018.03.009. Epub 2018 Mar 19. Spine J. 2018. PMID: 29567517
-
Biomechanical Changes of Adjacent and Fixed Segments Through Cortical Bone Trajectory Screw Fixation versus Traditional Trajectory Screw Fixation in the Lumbar Spine: A Finite Element Analysis.World Neurosurg. 2021 Jul;151:e447-e456. doi: 10.1016/j.wneu.2021.04.061. Epub 2021 Apr 22. World Neurosurg. 2021. PMID: 33895371
-
[Biomechanics of the bone-screw interface in transpedicular spinal instrumentation].Acta Ortop Mex. 2022 May-Jun;36(3):172-178. Acta Ortop Mex. 2022. PMID: 36862932 Review. Spanish.
-
A meta-analysis of complications associated with the use of cement-augmented pedicle screws in osteoporosis of spine.Orthop Traumatol Surg Res. 2021 Nov;107(7):102791. doi: 10.1016/j.otsr.2020.102791. Epub 2020 Dec 15. Orthop Traumatol Surg Res. 2021. PMID: 33338677 Review.
Cited by
-
Biomechanical Effect of Different Posterior Fixation Techniques on Stability and Adjacent Segment Degeneration in Treating Thoracolumbar Burst Fracture With Osteoporosis: A Finite Element Analysis.Spine (Phila Pa 1976). 2024 Aug 1;49(15):E229-E238. doi: 10.1097/BRS.0000000000005034. Epub 2024 May 9. Spine (Phila Pa 1976). 2024. PMID: 38721831 Free PMC article.
-
Finite element analysis of short-segment fixation combined with expandable polyetheretherketone vertebral body replacement in osteoporotic vertebrae.BMC Musculoskelet Disord. 2025 Aug 20;26(1):806. doi: 10.1186/s12891-025-09065-1. BMC Musculoskelet Disord. 2025. PMID: 40830948 Free PMC article.
-
Biomechanical comparison between unilateral and bilateral percutaneous vertebroplasty for osteoporotic vertebral compression fractures: A finite element analysis.Front Bioeng Biotechnol. 2022 Sep 8;10:978917. doi: 10.3389/fbioe.2022.978917. eCollection 2022. Front Bioeng Biotechnol. 2022. PMID: 36159704 Free PMC article.
-
Impact of cage position on biomechanical performance of stand-alone lateral lumbar interbody fusion: a finite element analysis.BMC Musculoskelet Disord. 2022 Oct 18;23(1):920. doi: 10.1186/s12891-022-05873-x. BMC Musculoskelet Disord. 2022. PMID: 36258213 Free PMC article.
-
Static study and numerical simulation of the influence of cement distribution in the upper and lower adjacent vertebrae on sandwich vertebrae in osteoporotic patients: Finite element analysis.JOR Spine. 2024 Jun 21;7(2):e1343. doi: 10.1002/jsp2.1343. eCollection 2024 Jun. JOR Spine. 2024. PMID: 38911099 Free PMC article.
References
-
- Shirahata T, Okano I, Salzmann SN, Sax OC, Shue J, Sama AA, et al. The Association between Surgical Level and Early Postoperative Thigh Symptoms among Patients Undergoing Standalone Lateral Lumbar Interbody Fusion (LLIF). World Neurosurg. 2019. 10.1016/j.wneu.2019.11.025. - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

