Association between mild stimulated IVF/M cycle and early embryo arrest in sub fertile women with/without PCOS
- PMID: 32669130
- PMCID: PMC7362506
- DOI: 10.1186/s12958-020-00622-y
Association between mild stimulated IVF/M cycle and early embryo arrest in sub fertile women with/without PCOS
Abstract
Background: The in vitro maturation (IVM) technique has physical and financial benefits, but a lower efficiency and outcome that is still unclear whether it is related to polycystic ovary syndrome (PCOS) itself or the IVM procedure. In this study, we analyzed the clinical and laboratory outcomes of an optimized IVM protocol in patients with and without PCOS. We also discussed the possible reasons for early embryo arrest in the IVM cycle.
Methods: This prospective study involved 58 PCOS patients and 56 non-PCOS patients who underwent mild stimulated IVF combined IVM (IVF/M) cycles. The clinical and laboratory outcomes were compared between the two groups. Also, metaphase II (MII) oocytes were obtained after IVM from the two groups, and in vivo MII oocytes randomly collected from IVF patients were examined for mitochondrial function using a laser scanning confocal microscope (LSCM). The aneuploidy rate for arrested cleavage embryos from IVM and IVF oocytes were screened using Next Generation Sequencing (NGS).
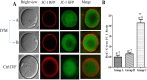
Results: Mildly stimulated IVF/M resulted in cumulative clinical pregnancy and implantation rates (40.2, 28.7% in the PCOS group vs. 41.9, 36% in the non-PCOS group), respectively. The blastocyst formation rates were comparable (28% vs. 28.2%) in PCOS and non-PCOS groups, respectively. Using LSCM, there was a significant decrease in the mitochondrial membrane potential of IVM oocytes compared with the control IVF oocytes (P < 0.001), but no significant difference between the PCOS and non-PCOS groups. The NGS showed that the aneuploidy rates were comparable (75, 75, and 66.6%) in IVM-PCOS, IVM-non-PCOS, and control IVF arrested embryos, respectively.
Conclusions: The mildly stimulated IVF/M protocol produced acceptable clinical outcomes in PCOS and non-PCOS patients. IVM itself rather than the PCOS condition adversely affected the embryo development through its effect on mitochondrial function, which appeared to be a possible cause for the embryo arrest in the IVM cycles rather than chromosomal aneuploidy.
Keywords: Aneuploidy; Embryo arrest; IVM; Mitochondria.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures

References
-
- Dahan MH, Tan SL, Chung J, Son WY. Clinical definition paper on in vitro maturation of human oocytes. Hum Reprod. 2016;31:1383–1386. - PubMed
-
- Chian RC, Buckett WM, Abdul Jalil AK, Son WY, Sylvestre C, Rao D, Tan SL. Natural-cycle in vitro fertilization combined with in vitro maturation of immature oocytes is a potential approach in infertility treatment. Fertil Steril. 2004;82:1675–1678. - PubMed
-
- Lim JH, Yang SH, Chian RC. New alternative to infertility treatment for women without ovarian stimulation. Reprod BioMed Online. 2007;14:547–549. - PubMed
-
- Son WY, Tan SL. Laboratory and embryological aspects of hCG-primed in vitro maturation cycles for patients with polycystic ovaries. Hum Reprod Update. 2010;16:675–689. - PubMed
-
- Chian RC, Lim JH, Tan SL. State of the art in in-vitro oocyte maturation. Curr Opin Obstet Gynecol. 2004;16:211–219. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

