The Comparison of HHHFNC and NCPAP in Extremely Low-Birth-Weight Preterm Infants After Extubation: A Single-Center Randomized Controlled Trial
- PMID: 32670991
- PMCID: PMC7332541
- DOI: 10.3389/fped.2020.00250
The Comparison of HHHFNC and NCPAP in Extremely Low-Birth-Weight Preterm Infants After Extubation: A Single-Center Randomized Controlled Trial
Abstract
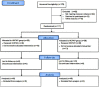
Objectives: To compare the clinical efficacy of heated, humidified high-flow nasal cannula (HHHFNC) and nasal continuous positive airway pressure (NCPAP) in extremely low-birth-weight preterm infants (ELBWI) after extubation. Methods: This trial included 94 extremely low-birth-weight infants (ELBWI), within 7 days after birth, and prepared for tracheal extubation and a change to non-invasive ventilation in the neonatal intensive care unit (NICU) admitted to our hospital from January 2015 to December 2018, with 48 infants in the HHHFNC group and 46 infants in the NCPAP group. Reintubation rate within 72 h after initial extubation, total ventilation time, non-invasive ventilation time, total oxygen inhalation time, and the time to reach full enteral feeding were the primary outcome measures. Total intestinal feeding time, average weight gain rate, days of hospitalization, costs of hospitalization, and complication rates, including nasal injury, IVH, BPD, NEC, ROP, and PDA, were used as secondary outcomes. Data were analyzed using Student's t-test or the Mann-Whitney U-test with a Chi-square test or Fisher's exact test, as appropriate, in SPSS (25.0). Results: HHHFNC not only shortened the oxygen exposure time but also effectively reduced the incidence of nasal injury (6.25 vs. 36.96%) and NEC (10.42 vs. 28.26%) (P < 0.05). Additionally, HHHFNC achieved a significant advance in the time to reach full enteral feeding (31.24 ± 11.35 vs. 34.21 ± 14.09 days); increased the average weight gain rate (16.07 ± 3.10 vs. 13.74 ± 4.21) and reduced the days of hospitalization (73.45 ± 18.84 vs. 79.24 ± 19.75), with a lower cost of hospitalization (16.04 ± 3.64 vs.18.79 ± 4.13) thousand dollars (all P < 0.05). Conclusions: Compared with NCPAP, HHHFNC was effective in preventing extubation failure in mechanically ventilated preterm ELBWI. HHHFNC shortens oxygen consumption time and significantly reduces the incidence of nasal injury and necrotizing enterocolitis; moreover, it can also reduce the length of stay and the hospitalization costs.
Keywords: extremely low-birth-weight preterm infants; heated humidified high-flow nasal cannula; nasal continuous positive airway pressure; preterm infant; respiratory distress syndrome.
Copyright © 2020 Chen, Lin, Du, Kang, Chi, Wang, Liu, Gao, Yang and Chen.
Figures
References
-
- Friedman CA, Menchaca RC, Baker MC, Rivas CK, Laberge RN, Rios EH, et al. . Bubble nasal CPAP, early surfactant treatment, and rapid extubation are associated with decreased incidence of bronchopulmonary dysplasia in very-low-birth-weight newborns: efficacy and safety considerations. Respir Care. (2013) 58:1134–42. 10.4187/respcare.01998 - DOI - PubMed
-
- Walsh BK, Brooks TM, Grenier BM. Oxygen therapy in the neonatal care environment. Respir Care. (2009) 54:1193–202. - PubMed
LinkOut - more resources
Full Text Sources