Internal Fixation versus Hemiarthroplasty in the Treatment of Unstable Intertrochanteric Fractures in the Elderly: A Systematic Review and Meta-Analysis
- PMID: 32691520
- PMCID: PMC7454150
- DOI: 10.1111/os.12736
Internal Fixation versus Hemiarthroplasty in the Treatment of Unstable Intertrochanteric Fractures in the Elderly: A Systematic Review and Meta-Analysis
Abstract
Objective: To evaluate the clinical efficacy of internal fixation versus hemiarthroplasty in the treatment of unstable intertrochanteric fractures in the elderly.
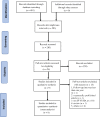
Methods: A search was conducted in PubMed, Web of Science, Embase, and Cochrane Library databases up to April 2020. The present study compared internal fixation and hemiarthroplasty in the treatment of unstable intertrochanteric fractures in the elderly. RevMan5.3 software provided by the International Cochrane Group was used for the meta-analysis. To compare the differences in the operation time, intraoperative bleeding, length of hospital stay, superficial infection, Harris hip score, mortality within 1 year, mortality within 2 years, reoperation, incidence of deep venous thrombosis (DVT), partial weight-bearing time, non-union, and implant-related complications between an internal fixation group and an hemiarthroplasty group.
Results: A total of 1300 patients were included in nine studies. The results showed that the operation time (MD = -18.09, 95% CI: -27.85--8.34, P = 0.0003), intraoperative bleeding (MD = -195.31, 95% CI: -244.8--147.74, P < 0.0001), implant-related complications (MD = 3.83, 95% CI: 1.74-8.45, P = 0.0008), and partial weight-bearing time (MD = 17.21, 95% CI: 1.63-32.79, P = 0.03) have statistical significance. However, there is not statistical significance for the Harris hip joint function scale (HHS) (MD = 5.60, 95% CI: -1.13-12.33, P = 0.10), DVT (MD = 1.02, 95% CI: 0.45-2.27, P = 0.97), length of hospital stay (MD = -1.08, 95% CI: -2.82-0.66, P = 0.22), superficial Infection (OR = 0.92, 95% CI: 0.43-1.98, P = 0.89), mortality within 1 year (OR = 0.95, 95% CI: 0.61-1.48, P = 0.81), mortality within 2 years (OR = 0.93, 95% CI: 0.61-1.43, P = 0.75), reoperation (MD = 1.80, 95% CI: 0.64-5.04, P = 0.26), and non-union (OR = 1.20, 95% CI: 0.48-3.03, P = 0.70). The result of the subgroup analysis showed no significant differences between the less than 2 years follow-up and the 2 years or more follow-up group. The only difference was for the Harris hip score: the internal fixation group was superior to the hemiarthroplasty group in the less than 2 years subgroup analysis, while there was no difference between the internal fixation group hemiarthroplasty group in the 2 years or more subgroup analysis.
Conclusion: Compared with the internal fixation group, those in the hemiarthroplasty group could carry out weight-bearing training early and implant-related complications were reduced, but it requires longer operation time and there is greater intraoperative blood loss. There is no difference in mortality, the incidence of DVT, non-union, HHS, reoperation, length of hospital stay, and superficial infection. Hemiarthroplasty may be a better choice for unstable intertrochanteric fractures in the elderly.
Keywords: Elderly; Hemiarthroplasty; Hip fractures; Internal fixators; Meta-analysis.
© 2020 The Authors. Orthopaedic Surgery published by Chinese Orthopaedic Association and John Wiley & Sons Australia, Ltd.
Figures







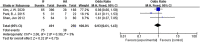





Similar articles
-
Proximal femoral nailing is superior to hemiarthroplasty in AO/OTA A2 and A3 intertrochanteric femur fractures in the elderly: a systematic literature review and meta-analysis.Int Orthop. 2020 Apr;44(4):623-633. doi: 10.1007/s00264-019-04351-9. Epub 2019 Jun 14. Int Orthop. 2020. PMID: 31201487
-
The choice of screw internal fixation and hemiarthroplasty in the treatment of femoral neck fractures in the elderly: a meta-analysis.J Orthop Surg Res. 2020 Sep 21;15(1):433. doi: 10.1186/s13018-020-01958-2. J Orthop Surg Res. 2020. PMID: 32958029 Free PMC article. Review.
-
A comparison of hemiarthroplasty versus dynamic hip screw fixation for intertrochanteric femoral fractures: a systematic review.Hip Int. 2023 Jul;33(4):752-761. doi: 10.1177/11207000221112579. Epub 2022 Jul 17. Hip Int. 2023. PMID: 35848138
-
[Proximal femoral nails antirotation and dynamic hip screws for fixation of unstable intertrochanteric fractures of femur: A meta-analysis].Beijing Da Xue Xue Bao Yi Xue Ban. 2019 Jun 18;51(3):493-500. doi: 10.19723/j.issn.1671-167X.2019.03.017. Beijing Da Xue Xue Bao Yi Xue Ban. 2019. PMID: 31209421 Free PMC article. Chinese.
-
Proximal femoral nails antirotation, Gamma nails, and dynamic hip screws for fixation of intertrochanteric fractures of femur: A meta-analysis.Orthop Traumatol Surg Res. 2014 Dec;100(8):859-66. doi: 10.1016/j.otsr.2014.07.023. Epub 2014 Nov 6. Orthop Traumatol Surg Res. 2014. PMID: 25453927
Cited by
-
Complication Rates and Survival of Nonagenarians after Hip Hemiarthroplasty versus Proximal Femoral Nail Antirotation for Intertrochanteric Fractures: A 15-Year Retrospective Cohort Study of 113 Cases.Orthop Surg. 2023 Dec;15(12):3231-3242. doi: 10.1111/os.13913. Epub 2023 Oct 25. Orthop Surg. 2023. PMID: 37880497 Free PMC article.
-
Hip Fractures in Malta: Does Delay in Surgery Affect Clinical Outcomes?Cureus. 2024 Dec 10;16(12):e75467. doi: 10.7759/cureus.75467. eCollection 2024 Dec. Cureus. 2024. PMID: 39791036 Free PMC article.
-
Continuous peripheral nerve block in patients with proximal femur fracture: A randomised comparison of three techniques.Indian J Anaesth. 2025 Apr;69(4):335-342. doi: 10.4103/ija.ija_1095_24. Epub 2025 Mar 13. Indian J Anaesth. 2025. PMID: 40687966 Free PMC article.
-
Treatment of Intertrochanteric Femur Fractures with Hip Arthroplasty in Older Patients: A Narrative Review of Indications and Outcomes.Medicina (Kaunas). 2021 Jul 27;57(8):763. doi: 10.3390/medicina57080763. Medicina (Kaunas). 2021. PMID: 34440969 Free PMC article. Review.
-
Computer-assisted cannulated screw internal fixation versus conventional cannulated screw internal fixation for femoral neck fractures: a systematic review and meta-analysis.J Orthop Surg Res. 2021 Nov 22;16(1):687. doi: 10.1186/s13018-021-02806-7. J Orthop Surg Res. 2021. PMID: 34809649 Free PMC article.
References
-
- Veronese N, Maggi S. Epidemiology and social costs of hip fracture. Injury, 2018, 49: 1458–1460. - PubMed
-
- Mazzucchelli Esteban R, Perez‐Fernandez E, Crespi‐Villarias N, et al Trends in osteoporotic hip fracture epidemiology over a 17‐year period in a spanish population: Alcorcon 1999‐2015. Arch Osteoporos, 2017, 12: 84. - PubMed
-
- Camurcu Y, Cobden A, Sofu H, et al What are the determinants of mortality after cemented bipolar hemiarthroplasty for unstable intertrochanteric fractures in elderly patients?. J Arthroplasty, 2017, 32: 3038–3043. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

