Pathophysiology and Acute Management of Tachyarrhythmias in Pheochromocytoma: JACC Review Topic of the Week
- PMID: 32703516
- PMCID: PMC7454044
- DOI: 10.1016/j.jacc.2020.04.080
Pathophysiology and Acute Management of Tachyarrhythmias in Pheochromocytoma: JACC Review Topic of the Week
Abstract
Pheochromocytomas, arising from chromaffin cells, produce catecholamines, epinephrine and norepinephrine. The tumor biochemical phenotype is defined by which of these exerts the greatest influence on the cardiovascular system when released into circulation in high amounts. Action on the heart and vasculature can cause potentially lethal arrhythmias, often in the setting of comorbid blood pressure derangements. In a review of electrocardiograms obtained on pheochromocytoma patients (n = 650) treated at our institution over the last decade, severe and refractory sinus tachycardia, atrial fibrillation, and ventricular tachycardia were found to be the most common or life-threatening catecholamine-induced tachyarrhythmias. These arrhythmias, arising from catecholamine excess rather than from a primary electrophysiologic substrate, require special considerations for treatment and complication avoidance. Understanding the synthesis and release of catecholamines, the adrenoceptors catecholamines bind to, and the cardiac and vascular response to epinephrine and norepinephrine underlies optimal management in catecholamine-induced tachyarrhythmias.
Keywords: blood pressure; catecholamines; pheochromocytoma; sinus tachycardia; tachyarrhythmias; ventricular tachycardia.
Copyright © 2020 American College of Cardiology Foundation. Published by Elsevier Inc. All rights reserved.
Figures







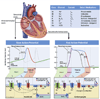
References
-
- Lenders JW, Eisenhofer G, Mannelli M, Pacak K. Phaeochromocytoma. Lancet 2005;366:665–75. - PubMed
-
- Sutton MG, Sheps SG, Lie JT. Prevalence of clinically unsuspected pheochromocytoma. Review of a 50-year autopsy series. Mayo Clin Proc 1981;56:354–60. - PubMed
-
- Stolk R, Bakx C, Mulder J, Timmers H, Lenders J. Is the excess cardiovascular morbidity in pheochromocytoma related to blood pressure or to catecholamines? J Clin Endocrinol Metab 2013;98:1100–6. - PubMed
-
- Prejbisz A, Lenders JWM, Eisenhofer G, Januszewicz A. Mortality associated with phaeochromocytoma. Horm Metab Res 2013;45:154–8. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

