Type 1 diabetes in Africa: an immunogenetic study in the Amhara of North-West Ethiopia
- PMID: 32705316
- PMCID: PMC7476916
- DOI: 10.1007/s00125-020-05229-x
Type 1 diabetes in Africa: an immunogenetic study in the Amhara of North-West Ethiopia
Abstract
Aims/hypothesis: We aimed to characterise the immunogenic background of insulin-dependent diabetes in a resource-poor rural African community. The study was initiated because reports of low autoantibody prevalence and phenotypic differences from European-origin cases with type 1 diabetes have raised doubts as to the role of autoimmunity in this and similar populations.
Methods: A study of consecutive, unselected cases of recently diagnosed, insulin-dependent diabetes (n = 236, ≤35 years) and control participants (n = 200) was carried out in the ethnic Amhara of rural North-West Ethiopia. We assessed their demographic and socioeconomic characteristics, and measured non-fasting C-peptide, diabetes-associated autoantibodies and HLA-DRB1 alleles. Leveraging genome-wide genotyping, we performed both a principal component analysis and, given the relatively modest sample size, a provisional genome-wide association study. Type 1 diabetes genetic risk scores were calculated to compare their genetic background with known European type 1 diabetes determinants.
Results: Patients presented with stunted growth and low BMI, and were insulin sensitive; only 15.3% had diabetes onset at ≤15 years. C-peptide levels were low but not absent. With clinical diabetes onset at ≤15, 16-25 and 26-35 years, 86.1%, 59.7% and 50.0% were autoantibody positive, respectively. Most had autoantibodies to GAD (GADA) as a single antibody; the prevalence of positivity for autoantibodies to IA-2 (IA-2A) and ZnT8 (ZnT8A) was low in all age groups. Principal component analysis showed that the Amhara genomes were distinct from modern European and other African genomes. HLA-DRB1*03:01 (p = 0.0014) and HLA-DRB1*04 (p = 0.0001) were positively associated with this form of diabetes, while HLA-DRB1*15 was protective (p < 0.0001). The mean type 1 diabetes genetic risk score (derived from European data) was higher in patients than control participants (p = 1.60 × 10-7). Interestingly, despite the modest sample size, autoantibody-positive patients revealed evidence of association with SNPs in the well-characterised MHC region, already known to explain half of type 1 diabetes heritability in Europeans.
Conclusions/interpretation: The majority of patients with insulin-dependent diabetes in rural North-West Ethiopia have the immunogenetic characteristics of autoimmune type 1 diabetes. Phenotypic differences between type 1 diabetes in rural North-West Ethiopia and the industrialised world remain unexplained.
Keywords: Africa; Autoantibodies; Ethiopia; Genomes; HLA; Rural; Type 1 diabetes.
Figures

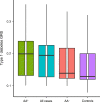
References
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials

