Cardiovascular changes during peanut-induced allergic reactions in human subjects
- PMID: 32707226
- PMCID: PMC7858218
- DOI: 10.1016/j.jaci.2020.06.033
Cardiovascular changes during peanut-induced allergic reactions in human subjects
Abstract
Background: Food allergy is the most common cause of anaphylaxis. Changes in posture during acute reactions can trigger fatal outcomes, but the impact of allergic reactions on the cardiovascular system in nonfatal reactions remains poorly understood.
Objective: Our aim was to systematically evaluate changes in cardiovascular function during acute allergic reactions to peanut.
Methods: Participants underwent double-blind placebo-controlled food challenge to peanut as part of a clinical trial. Changes in hemodynamic parameters (heart rate, stroke volume, blood pressure, and peripheral blood flow) and electrocardiogram findings during food challenges were assessed using noninvasive continuous monitoring.
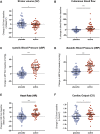
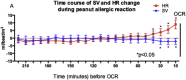
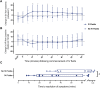
Results: A total of 57 adults (median age 24 years [interquartile range = 20-29]), 53% of whom were female, participated; 22 (39%) had anaphylaxis. Acute reactions were associated with significant changes in stroke volume (mean decrease of 4.2% [95% CI = 0.8-7.6; P = .03]), heart rate (mean increase 11.6% [95% CI = 8.4-14.8; P < .0001]), and peripheral blood flow (mean increase 19.7% [95% CI = 10.8-28.6; P < .0001]), irrespective of reaction severity. These changes were reproduced at a subsequent repeat peanut challenge in 26 participants, and could be reversed with administration of intravenous fluids which resulted in faster resolution of abdominal symptoms.
Conclusions: In this first detailed human study of cardiovascular changes during food-induced allergic reactions, we found evidence for significant fluid redistribution, independent of reaction severity. This provides a sound rationale for optimizing venous return during significant allergic reactions to food. Finally, these data provide a new paradigm for understanding severity in anaphylaxis, in which poor outcomes may occur as a result of a failure in compensatory mechanisms.
Keywords: Anaphylaxis; cardiac output; cardiovascular; food allergens; intravenous fluids; management; stroke volume; venous return.
Copyright © 2020 The Authors. Published by Elsevier Inc. All rights reserved.
Figures




References
-
- Vigorito C., Giordano A., De Caprio L., Vitale D.F., Maurea N., Silvestri P. Effects of histamine on coronary hemodynamics in humans: role of H1 and H2 receptors. J Am Coll Cardiol. 1987;10:1207–1213. - PubMed
-
- Turner P.J., Baumert J.L., Beyer K., Boyle R.J., Chan C.H., Clark A.T. Can we identify patients at risk of life-threatening allergic reactions to food? Allergy. 2016;71:1241–1255. - PubMed
-
- Pumphrey R.S. Fatal posture in anaphylactic shock. J Allergy Clin Immunol. 2003;112:451–452. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

