Emtricitabine and tenofovir alafenamide vs emtricitabine and tenofovir disoproxil fumarate for HIV pre-exposure prophylaxis (DISCOVER): primary results from a randomised, double-blind, multicentre, active-controlled, phase 3, non-inferiority trial
- PMID: 32711800
- PMCID: PMC9665936
- DOI: 10.1016/S0140-6736(20)31065-5
Emtricitabine and tenofovir alafenamide vs emtricitabine and tenofovir disoproxil fumarate for HIV pre-exposure prophylaxis (DISCOVER): primary results from a randomised, double-blind, multicentre, active-controlled, phase 3, non-inferiority trial
Abstract
Background: Tenofovir alafenamide shows high antiviral efficacy and improved renal and bone safety compared with tenofovir disoproxil fumarate when used for HIV treatment. Here, we report primary results from a blinded phase 3 study evaluating the efficacy and safety of pre-exposure prophylaxis (PrEP) with emtricitabine and tenofovir alafenamide versus emtricitabine and tenofovir disoproxil fumarate for HIV prevention.
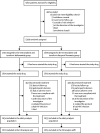
Methods: This study is an ongoing, randomised, double-blind, multicentre, active-controlled, phase 3, non-inferiority trial done at 94 community, public health, and hospital-associated clinics located in regions of Europe and North America, where there is a high incidence of HIV or prevalence of people living with HIV, or both. We enrolled adult cisgender men who have sex with men and transgender women who have sex with men, both with a high risk of acquiring HIV on the basis of their self-reported sexual behaviour in the past 12 weeks or their recent history (within 24 weeks of enrolment) of bacterial sexually transmitted infections. Participants with current or previous use of PrEP with emtricitabine and tenofovir disoproxil fumarate were not excluded. We used a computer-generated random allocation sequence to randomly assign (1:1) participants to receive either emtricitabine (200 mg) and tenofovir alafenamide (25 mg) tablets daily, with matched placebo tablets (emtricitabine and tenofovir alafenamide group), or emtricitabine (200 mg) and tenofovir disoproxil fumarate (300 mg) tablets daily, with matched placebo tablets (emtricitabine and tenofovir disoproxil fumarate group). As such, all participants were given two tablets. The trial sponsor, investigators, participants, and the study staff who provided the study drugs, assessed the outcomes, and collected the data were masked to group assignment. The primary efficacy outcome was incident HIV infection, which was assessed when all participants had completed 48 weeks of follow-up and half of all participants had completed 96 weeks of follow-up. This full analysis set included all randomly assigned participants who had received at least one dose of the assigned study drug and had at least one post-baseline HIV test. Non-inferiority of emtricitabine and tenofovir alafenamide to emtricitabine and tenofovir disoproxil fumarate was established if the upper bound of the 95·003% CI of the HIV incidence rate ratio (IRR) was less than the prespecified non-inferiority margin of 1·62. We prespecified six secondary bone mineral density and renal biomarker safety endpoints to evaluate using the safety analysis set. This analysis set included all randomly assigned participants who had received at least one dose of the assigned study drug. This trial is registered with ClinicalTrials.gov, NCT02842086, and is no longer recruiting.
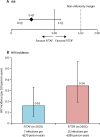
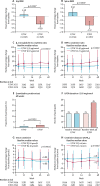
Findings: Between Sept 13, 2016, and June 30, 2017, 5387 (92%) of 5857 participants were randomly assigned and received emtricitabine and tenofovir alafenamide (n=2694) or emtricitabine and tenofovir disoproxil fumarate (n=2693). At the time of the primary efficacy analysis (ie, when all participants had completed 48 weeks and 50% had completed 96 weeks) emtricitabine and tenofovir alafenamide was non-inferior to emtricitabine and tenofovir disoproxil fumarate for HIV prevention, as the upper limit of the 95% CI of the IRR, was less than the prespecified non-inferiority margin of 1·62 (IRR 0·47 [95% CI 0·19-1·15]). After 8756 person-years of follow-up, 22 participants were diagnosed with HIV, seven participants in the emtricitabine and tenofovir alafenamide group (0·16 infections per 100 person-years [95% CI 0·06-0·33]), and 15 participants in the emtricitabine and tenofovir disoproxil fumarate group (0·34 infections per 100 person-years [0·19-0·56]). Both regimens were well tolerated, with a low number of participants reporting adverse events that led to discontinuation of the study drug (36 [1%] of 2694 participants in the emtricitabine and tenofovir alafenamide group vs 49 [2%] of 2693 participants in the emtricitabine and tenofovir disoproxil fumarate group). Emtricitabine and tenofovir alafenamide was superior to emtricitabine and tenofovir disoproxil fumarate in all six prespecified bone mineral density and renal biomarker safety endpoints.
Interpretation: Daily emtricitabine and tenofovir alafenamide shows non-inferior efficacy to daily emtricitabine and tenofovir disoproxil fumarate for HIV prevention, and the number of adverse events for both regimens was low. Emtricitabine and tenofovir alafenamide had more favourable effects on bone mineral density and biomarkers of renal safety than emtricitabine and tenofovir disoproxil fumarate.
Funding: Gilead Sciences.
Copyright © 2020 Elsevier Ltd. All rights reserved.
Figures
Comment in
-
DISCOVER: much accomplished, but not yet for all.Lancet. 2020 Jul 25;396(10246):214-215. doi: 10.1016/S0140-6736(20)31530-0. Lancet. 2020. PMID: 32711780 Free PMC article. No abstract available.
References
-
- Molina JM, Capitant C, Spire B, et al. On-demand preexposure prophylaxis in men at high risk for HIV-1 infection. N Engl J Med. 2015;373:2237–2246. - PubMed
Publication types
MeSH terms
Substances
Associated data
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

