Endoscopic and Surgical Treatments for Gastroparesis: What to Do and Whom to Treat?
- PMID: 32718569
- PMCID: PMC7391056
- DOI: 10.1016/j.gtc.2020.04.008
Endoscopic and Surgical Treatments for Gastroparesis: What to Do and Whom to Treat?
Abstract
Gastroparesis is a complex chronic debilitating condition of gastric motility resulting in the delayed gastric emptying and multiple severe symptoms, which may lead to malnutrition and dehydration. Initial management of patients with gastroparesis focuses on the diet, lifestyle modification and medical therapy. Various endoscopic and surgical interventions are reserved for refractory cases of gastroparesis, not responding to conservative therapy. Pyloric interventions, enteral access tubes, gastric electrical stimulator and gastrectomy have been described in the care of patients with gastroparesis. In this article, the authors review current management, indications, and contraindications to these procedures.
Keywords: Gastric electrical stimulator; Gastric pacemaker; Gastric peroral endoscopic myotomy (GPOEM); Gastroparesis; Peroral pyloromyotomy (POP); Pyloromyotomy; Pyloroplasty.
Copyright © 2020 Elsevier Inc. All rights reserved.
Conflict of interest statement
Disclosure Funded by: NIHHYB. Grant number(s): NIH/NCI Cancer Center Support Grant P30 CA006927. NIHMS-ID: 1591505.
Figures

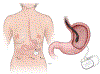







References
-
- Soykan I, Sivri B, Sarosiek I, Kiernan B, McCallum RW. Demography, clinical characteristics, psychological and abuse profiles, treatment, and long-term follow-up of patients with gastroparesis. Dig Dis Sci. 1998. November;43(11):2398–404. - PubMed
-
- Rabine JC, Barnett JL. Management of the patient with gastroparesis. J Clin Gastroenterol. 2001. January;32(1):11–8. - PubMed
-
- Pasricha PJ, Ravich WJ, Hendrix TR, Sostre S, Jones B, Kalloo AN. Intrasphincteric botulinum toxin for the treatment of achalasia. N Engl J Med. 1995. March 23;332(12):774–8. - PubMed
-
- Miller LS, Szych GA, Kantor SB, Bromer MQ, Knight LC, Maurer AH, et al. Treatment of idiopathic gastroparesis with injection of botulinum toxin into the pyloric sphincter muscle. Am J Gastroenterol. 2002. July;97(7):1653–60. - PubMed
-
- Lacy BE, Crowell MD, Schettler-Duncan A, Mathis C, Pasricha PJ. The treatment of diabetic gastroparesis with botulinum toxin injection of the pylorus. Diabetes Care. 2004. October;27(10):2341–7. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

