Clinical Significance of Electronegative Low-Density Lipoprotein Cholesterol in Atherothrombosis
- PMID: 32751498
- PMCID: PMC7460408
- DOI: 10.3390/biomedicines8080254
Clinical Significance of Electronegative Low-Density Lipoprotein Cholesterol in Atherothrombosis
Abstract
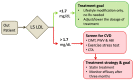
Despite the numerous risk factors for atherosclerotic cardiovascular diseases (ASCVD), cumulative evidence shows that electronegative low-density lipoprotein (L5 LDL) cholesterol is a promising biomarker. Its toxicity may contribute to atherothrombotic events. Notably, plasma L5 LDL levels positively correlate with the increasing severity of cardiovascular diseases. In contrast, traditional markers such as LDL-cholesterol and triglyceride are the therapeutic goals in secondary prevention for ASCVD, but that is controversial in primary prevention for patients with low risk. In this review, we point out the clinical significance and pathophysiological mechanisms of L5 LDL, and the clinical applications of L5 LDL levels in ASCVD can be confidently addressed. Based on the previously defined cut-off value by receiver operating characteristic curve, the acceptable physiological range of L5 concentration is proposed to be below 1.7 mg/dL. When L5 LDL level surpass this threshold, clinically relevant ASCVD might be present, and further exams such as carotid intima-media thickness, pulse wave velocity, exercise stress test, or multidetector computed tomography are required. Notably, the ultimate goal of L5 LDL concentration is lower than 1.7 mg/dL. Instead, with L5 LDL greater than 1.7 mg/dL, lipid-lowering treatment may be required, including statin, ezetimibe or PCSK9 inhibitor, regardless of the low-density lipoprotein cholesterol (LDL-C) level. Since L5 LDL could be a promising biomarker, we propose that a high throughput, clinically feasible methodology is urgently required not only for conducting a prospective, large population study but for developing therapeutics strategies to decrease L5 LDL in the blood.
Keywords: L5 LDL; LDL(–); atherosclerosis; cardiovascular disease; electronegative low-density lipoprotein; oxLDL; oxidized LDL.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

References
-
- Stone N.J., Robinson J.G., Lichtenstein A.H., Bairey Merz C.N., Blum C.B., Eckel R.H., Goldberg A.C., Gordon D., Levy D., Lloyd-Jones D.M., et al. 2013 ACC/AHA guideline on the treatment of blood cholesterol to reduce atherosclerotic cardiovascular risk in adults: A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J. Am. Coll. Cardiol. 2014;63:2889–2934. - PubMed
-
- Grundy S.M., Stone N.J., Bailey A.L., Beam C., Birtcher K.K., Blumenthal R.S., Braun L.T., de Ferranti S., Faiella-Tommasino J., Forman D.E., et al. 2018 AHA/ACC/AACVPR/AAPA/ABC/ACPM/ADA/AGS/APhA/ASPC/NLA/PCNA Guideline on the Management of Blood Cholesterol: Executive Summary: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. J. Am. Coll. Cardiol. 2019;73:3168–3209. doi: 10.1016/j.jacc.2018.11.002. - DOI - PubMed
-
- Mach F., Baigent C., Catapano A.L., Koskinas K.C., Casula M., Badimon L., Chapman M.J., De Backer G.G., Delgado V., Ference B.A., et al. 2019 ESC/EAS Guidelines for the management of dyslipidaemias: Lipid modification to reduce cardiovascular risk. Eur. Heart J. 2020;41:111–188. doi: 10.1093/eurheartj/ehz455. - DOI - PubMed
-
- Fernandez-Friera L., Fuster V., Lopez-Melgar B., Oliva B., Garcia-Ruiz J.M., Mendiguren J., Bueno H., Pocock S., Ibanez B., Fernandez-Ortiz A., et al. Normal LDL-Cholesterol Levels Are Associated With Subclinical Atherosclerosis in the Absence of Risk Factors. J. Am. Coll. Cardiol. 2017;70:2979–2991. doi: 10.1016/j.jacc.2017.10.024. - DOI - PubMed
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

