Could dementia be detected from UK primary care patients' records by simple automated methods earlier than by the treating physician? A retrospective case-control study
- PMID: 32766457
- PMCID: PMC7385545
- DOI: 10.12688/wellcomeopenres.15903.1
Could dementia be detected from UK primary care patients' records by simple automated methods earlier than by the treating physician? A retrospective case-control study
Abstract
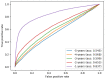
Background: Timely diagnosis of dementia is a policy priority in the United Kingdom (UK). Primary care physicians receive incentives to diagnose dementia; however, 33% of patients are still not receiving a diagnosis. We explored automating early detection of dementia using data from patients' electronic health records (EHRs). We investigated: a) how early a machine-learning model could accurately identify dementia before the physician; b) if models could be tuned for dementia subtype; and c) what the best clinical features were for achieving detection. Methods: Using EHRs from Clinical Practice Research Datalink in a case-control design, we selected patients aged >65y with a diagnosis of dementia recorded 2000-2012 (cases) and matched them 1:1 to controls; we also identified subsets of Alzheimer's and vascular dementia patients. Using 77 coded concepts recorded in the 5 years before diagnosis, we trained random forest classifiers, and evaluated models using Area Under the Receiver Operating Characteristic Curve (AUC). We examined models by year prior to diagnosis, subtype, and the most important features contributing to classification. Results: 95,202 patients (median age 83y; 64.8% female) were included (50% dementia cases). Classification of dementia cases and controls was poor 2-5 years prior to physician-recorded diagnosis (AUC range 0.55-0.65) but good in the year before (AUC: 0.84). Features indicating increasing cognitive and physical frailty dominated models 2-5 years before diagnosis; in the final year, initiation of the dementia diagnostic pathway (symptoms, screening and referral) explained the sudden increase in accuracy. No substantial differences were seen between all-cause dementia and subtypes. Conclusions: Automated detection of dementia earlier than the treating physician may be problematic, if using only primary care data. Future work should investigate more complex modelling, benefits of linking multiple sources of healthcare data and monitoring devices, or contextualising the algorithm to those cases that the GP would need to investigate.
Keywords: Dementia; diagnosis; early detection; electronic patient records; machine learning.; primary care.
Copyright: © 2020 Ford E et al.
Conflict of interest statement
No competing interests were disclosed.
Figures

References
-
- Prince M, Knapp M, Guerchet M, et al. : Dementia UK Update. London, UK;2014. Reference Source
-
- Prince M, Bryce R, Ferr C: Alzheimer's Disease International World Alzheimer Report 2011: The benefits of early diagnosis and intervention.Institute of Psychiatry King's College London Alzheimer's Disease International.2011. Reference Source
-
- Salib E, Thompson J: Use of anti-dementia drugs and delayed care home placement: an observational study. The Psychiatrist. 2011;35(10):384–8. 10.1192/pb.bp.110.033431 - DOI
-
- Department of Health: Living well with dementia: A National Dementia Strategy.2009. Reference Source
-
- Department of Health: Prime Minister’s challenge on dementia: Delivering major improvements in dementia care and research by 2015.2012. Reference Source
Grants and funding
LinkOut - more resources
Full Text Sources

