Factors influencing the length of hospital stay during the intensive phase of multidrug-resistant tuberculosis treatment at Amhara regional state hospitals, Ethiopia: a retrospective follow up study
- PMID: 32770982
- PMCID: PMC7414745
- DOI: 10.1186/s12889-020-09324-x
Factors influencing the length of hospital stay during the intensive phase of multidrug-resistant tuberculosis treatment at Amhara regional state hospitals, Ethiopia: a retrospective follow up study
Abstract
Background: The length of hospital stay is the duration of hospitalization, which reflects disease severity and resource utilization indirectly. Generally, tuberculosis is considered an ambulatory disease that could be treated at DOTs clinics; however, admission remains an essential component for patients' clinical stabilization. Hence, this study aimed to identify factors influencing hospital stay length during the intensive phase of multidrug-resistant tuberculosis treatment.
Methods: A retrospective follow-up study was conducted at three hospitals, namely the University of Gondar comprehensive specialized, Borumeda, and Debremarkos referral hospitals from September 2010 to December 2016 (n = 432). Data extracted from hospital admission/discharge logbooks and individual patient medical charts. A binary logistic regression analysis was used to identify factors associated with more extended hospital stays during the intensive phase of multidrug-resistant tuberculosis treatment.
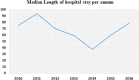
Result: Most patients (93.5%) had a pulmonary form of multidrug-resistant tuberculosis and 26.2% had /TB/HIV co-infections. The median length of hospital stays was 62 (interquartile range from 36 to 100) days. The pulmonary form of tuberculosis (Adjusted odds ratio [AOR], 3.47, 95% confidence interval [CI]; 1.31 to 9.16), bedridden functional status (AOR = 2.88, 95%CI; 1.29 to 6.43), and adverse drug effects (AOR = 2.11, 95%CI; 1.35 to 3.30) were factors associated with extended hospital stays.
Conclusion: This study revealed that the length of hospital-stay differed significantly between the hospitals. The pulmonary form of tuberculosis decreased functional status at admission and reported adverse drug reactions were determinants of more extended hospital stays. These underscore the importance of early case detection and prompt treatment of adverse drug effects.
Keywords: Ethiopia; Length of hospital stay; Multidrug-resistant tuberculosis.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
References
-
- World Health Organization, World Health Organization. Global tuberculosis report 2015. 2015.
-
- Rieu R, et al. Time to detection in liquid culture of sputum in pulmonary MDR-TB does not predict culture conversion for early discharge. J Antimicrob Chemother. 2015;1:dkv407. - PubMed
-
- Annabel B, Anna D, Hannah M. Global tuberculosis report 2019. Geneva: World Health Organization; 2019.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources