Clinical features of hemichoreahemiballism: A stroke-related movement disorder
- PMID: 32774821
- PMCID: PMC7378540
- DOI: 10.4081/ni.2020.8328
Clinical features of hemichoreahemiballism: A stroke-related movement disorder
Abstract
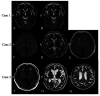
We examined pathogenesis and clinical features of three hemichorea-hemiballism (HCHB) cases. We studied their age, magnetic resonance imaging results, vascular risk factors, management, and outcomes. One man and two women (aged 74-86 years) demonstrated acute onset of HCHB, lasting for at least several months. Patients had one or more vascular risk factors, including hypertension and diabetes. All patients presented subacute or old infarction in the basal ganglia with contralateral symptoms. We administered clonazepam (0.5-1 mg/day), haloperidol (0.375-0.75 mg/day), or both as necessary and observed symptom-control. Vascular lesions in the basal ganglia were a contributing factor. Symptoms were controlled using pharmacotherapy with gamma-aminobutyric acid-agonist (clonazepam) or anti-dopaminergic (haloperidol) medication.
Keywords: Hemichorea-hemiballism; Strokerelated movement disorders; basal ganglia.
©Copyright: the Author(s).
Conflict of interest statement
Conflict of interest: The authors declare no conflicts of interest.
Figures

Similar articles
-
Hemichorea associated with ipsilateral basal ganglia lesions.Neurol Sci. 2025 Jun;46(6):2829-2831. doi: 10.1007/s10072-025-08059-0. Epub 2025 Mar 3. Neurol Sci. 2025. PMID: 40029542
-
Neuroradiological Evolution of Glycaemic Hemichorea-Hemiballism and the Possible Role of Brain Hypoperfusion.Eur J Case Rep Intern Med. 2019 Oct 23;6(11):001257. doi: 10.12890/2019_001257. eCollection 2019. Eur J Case Rep Intern Med. 2019. PMID: 31890704 Free PMC article.
-
A case of Hemichorea-Hemiballism Induced by Acute Infarction of Bilateral Corona Radiata and Cortex.Cell Biochem Biophys. 2015 Sep;73(1):171-4. doi: 10.1007/s12013-015-0608-6. Cell Biochem Biophys. 2015. PMID: 25707502
-
Pharmacological approaches to treatment of hemiballism and hemichorea.Brain Res Bull. 1983 Aug;11(2):187-9. doi: 10.1016/0361-9230(83)90189-2. Brain Res Bull. 1983. PMID: 6138134 Review.
-
[Hemichorea-hemiballism associated to basal ganglia hemorrhage in uncontrolled diabetes mellitus: report of two cases].Arq Neuropsiquiatr. 1996 Sep;54(3):461-5. doi: 10.1590/s0004-282x1996000300016. Arq Neuropsiquiatr. 1996. PMID: 9109992 Review. Portuguese.
References
-
- Mehanna R, Jankovic J. Movement disorders in cerebrovascular diseases. Lancet Neurol 2013;12:597-608. - PubMed
-
- Hashimoto T, Hanyu N, Yahikozawa H, Yanagisawa N. Persistent hemiballism with striatal hyperintensity on T1- weighted MRI in a diabetic patient: a 6-year follow-up study. J Neurol Sci 1999;165:178-81. - PubMed
LinkOut - more resources
Full Text Sources
