Predictors for the development of preoperative oxygenation impairment in acute aortic dissection in hypertensive patients
- PMID: 32778051
- PMCID: PMC7416810
- DOI: 10.1186/s12872-020-01652-5
Predictors for the development of preoperative oxygenation impairment in acute aortic dissection in hypertensive patients
Abstract
Background: Acute aortic dissection (AAD) is an acute life-threatening cardiovascular disease, which is frequently complicated with oxygenation impairment (OI). We aim to investigate predictors of the development of OI in the patients with AAD.
Methods: We retrospectively collected clinical data of AAD in hypertensive patients from July 2012 to March 2020. The patients included in this study were divided into OI (+) group (oxygenation index≤200) and OI (-) group (oxygenation index> 200). Both groups were compared according to demographic and clinical characteristics, and laboratory findings. Characteristics of hypertension in the patients with AAD were described. Predictors for the development of OI were assessed. And cutoff values were determined by receiver operating characteristics (ROC) curve.
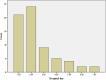
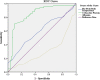
Results: A total of 208 patients were included in this study and the incidence of OI was 32.2%. In OI (+) group, patients had significantly higher peak body temperature (37.85 ± 0.60 vs 37.64 ± 0.44 °C, P = .005), higher levels of CRP (42.70 ± 28.27 vs 13.90 ± 18.70 mg/L, P = .000) and procalcitonin (1.07 ± 3.92 vs 0.31 ± 0.77μg/L, P = .027), and lower levels of albumin (34.21 ± 5.65 vs 37.73 ± 4.70 g/L, P = .000). Spearman's rank correlation test showed that the minimum oxygenation index was positively correlated with albumin, and was negatively correlated with the peak body temperature, serum CRP, procalcitonin, BNP and troponin. The stepwise multiple linear regression analysis showed that the peak body temperature, serum CRP and albumin were independently associated with development of OI. An optimal cutoff value for CRP for predicting OI was ≥9.20 mg/L, with a sensitivity of 91.0% and a specificity of 61.0%.
Conclusions: The peak body temperature, serum CRP and albumin were independent predictors of OI development in the patients with AAD. The serum CRP on admission≥9.20 mg/L might be a valuable and reliable indicator in predicting the development of OI.
Keywords: Acute aortic dissection; Albumin; C-reactive protein; Oxygenation impairment; Systemic inflammatory response syndrome.
Conflict of interest statement
There is no conflict of interest to declare in this study.
Figures
Similar articles
-
Serum C-reactive protein elevation predicts poor clinical outcome in patients with distal type acute aortic dissection: association with the occurrence of oxygenation impairment.Int J Cardiol. 2005 Jun 22;102(1):39-45. doi: 10.1016/j.ijcard.2004.03.076. Int J Cardiol. 2005. PMID: 15939097
-
Reduction of the PaO2/FiO2 ratio in acute aortic dissection – relationship between the extent of dissection and inflammation –.Circ J. 2010 Oct;74(10):2066-73. doi: 10.1253/circj.cj-10-0336. Epub 2010 Aug 6. Circ J. 2010. PMID: 20697178
-
Value of C-reactive protein/albumin ratio in predicting the development of preoperative oxygenation impairment in patients with Stanford type-B acute aortic dissection.Int J Cardiol Heart Vasc. 2024 Jan 11;50:101337. doi: 10.1016/j.ijcha.2024.101337. eCollection 2024 Feb. Int J Cardiol Heart Vasc. 2024. PMID: 38282751 Free PMC article.
-
Prognostic Role of Admission C-Reactive Protein Level as a Predictor of In-Hospital Mortality in Type-A Acute Aortic Dissection: A Meta-Analysis.Vasc Endovascular Surg. 2019 Oct;53(7):547-557. doi: 10.1177/1538574419858161. Epub 2019 Jun 27. Vasc Endovascular Surg. 2019. PMID: 31248351
-
Admission C-reactive protein and outcomes in acute aortic dissection: a systematic review.Croat Med J. 2019 Aug 31;60(4):309-315. doi: 10.3325/cmj.2019.60.309. Croat Med J. 2019. PMID: 31483116 Free PMC article.
Cited by
-
Perioperative oxygenation impairment related to type a aortic dissection.Perfusion. 2025 Jan;40(1):49-60. doi: 10.1177/02676591231224997. Epub 2024 Jan 4. Perfusion. 2025. PMID: 38174389 Free PMC article. Review.
-
Preoperative acute lung injury and oxygenation impairment occurred in the patients with acute aortic dissection.BMC Cardiovasc Disord. 2022 Mar 27;22(1):129. doi: 10.1186/s12872-022-02579-9. BMC Cardiovasc Disord. 2022. PMID: 35346059 Free PMC article. Review.
-
Non-invasive positive pressure ventilation can reduce perioperative mortality in acute aortic dissection patients with hypoxemia.J Thorac Dis. 2024 Sep 30;16(9):5835-5845. doi: 10.21037/jtd-24-163. Epub 2024 Sep 19. J Thorac Dis. 2024. PMID: 39444862 Free PMC article.
-
The Incidence, Risk Factors, and Hospital Mortality of Prolonged Mechanical Ventilation among Cardiac Surgery Patients: A Systematic Review and Meta-Analysis.Rev Cardiovasc Med. 2024 Nov 20;25(11):409. doi: 10.31083/j.rcm2511409. eCollection 2024 Nov. Rev Cardiovasc Med. 2024. PMID: 39618849 Free PMC article.
-
Single-Cell RNA Sequencing Reveals Smooth Muscle Cells Heterogeneity in Experimental Aortic Dissection.Front Genet. 2022 Aug 11;13:836593. doi: 10.3389/fgene.2022.836593. eCollection 2022. Front Genet. 2022. PMID: 36035191 Free PMC article.
References
-
- Gawinecka J, Schonrath F, von Eckardstein A. Acute aortic dissection: pathogenesis, risk factors and diagnosis. Swiss Med Wkly. 2017;147:w14489. - PubMed
-
- Nienaber CA, Clough RE, Sakalihasan N, Suzuki T, Gibbs R, Mussa F, et al. Aortic dissection. Nat Rev Dis Primers. 2016;2:16053. - PubMed
-
- Hasegawa Y, Ishikawa S, Ohtaki A, Otani Y, Takahashi T, Sato Y, et al. Impaired lung oxgenation in acute aortic dissection. J Cardiovasc Surg. 1999;40(2):191–195. - PubMed
-
- Sugano Y, Anzai T, Yoshikawa T, Satoh T, Iwanaga S, Hayashi T, et al. Serum C-reactive protein elevation predicts poor clinical outcome in patients with distal type acute aortic dissection: association with the occurrence of oxygenation impairment. Int J Cardiol. 2005;102(1):39–45. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

