Obesity as a contributor to immunopathology in pregnant and non-pregnant adults with COVID-19
- PMID: 32779790
- PMCID: PMC7435524
- DOI: 10.1111/aji.13320
Obesity as a contributor to immunopathology in pregnant and non-pregnant adults with COVID-19
Abstract
The ongoing coronavirus disease 2019 (COVID-19) pandemic has led to a global public health emergency with the need to identify vulnerable populations who may benefit from increased screening and healthcare resources. Initial data suggest that overall, pregnancy is not a significant risk factor for severe coronavirus disease 2019 (COVID-19). However, case series have suggested that maternal obesity is one of the most important comorbidities associated with more severe disease. In obese individuals, suppressors of cytokine signaling are upregulated and type I and III interferon responses are delayed and blunted leading to ineffective viral clearance. Obesity is also associated with changes in systemic immunity involving a wide range of immune cells and mechanisms that lead to low-grade chronic inflammation, which can compromise antiviral immunity. Macrophage activation in adipose tissue can produce low levels of pro-inflammatory cytokines (TNF-α, IL-1β, IL-6). Further, adipocyte secretion of leptin is pro-inflammatory and high circulating levels of leptin have been associated with mortality in patients with acute respiratory distress syndrome. The synergistic effects of obesity-associated delays in immune control of COVID-19 with mechanical stress of increased adipose tissue may contribute to a greater risk of pulmonary compromise in obese pregnant women. In this review, we bring together data regarding obesity as a key co-morbidity for COVID-19 in pregnancy with known changes in the antiviral immune response associated with obesity. We also describe how the global burden of obesity among reproductive age women has serious public health implications for COVID-19.
Keywords: COVID-19; maternal health; obesity; pneumonia; pregnancy.
© 2020 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd.
Figures

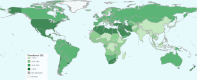
References
-
- Coronavirus Disease 2019 (COVID‐19): people with certain medical conditions. 2020; https://www.cdc.gov/coronavirus/2019‐ncov/need‐extra‐precautions/people‐.... Accessed July 29, 2020.
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources

