Advanced cardiac magnetic resonance imaging in takotsubo cardiomyopathy
- PMID: 32795180
- PMCID: PMC8519651
- DOI: 10.1259/bjr.20200514
Advanced cardiac magnetic resonance imaging in takotsubo cardiomyopathy
Abstract
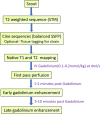
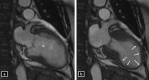
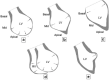
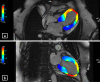
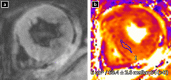
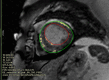
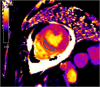
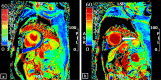
Takotsubo cardiomyopathy (TC) is a reversible condition in which there is transient left ventricular (LV) dysfunction characterised most commonly by basal hyperkinesis and mid-apical LV ballooning and hypokinesia. It is said to be triggered by stress and mimics, such as acute coronary syndrome (ACS) clinically. Diagnosis is usually suspected on echocardiography due to the characteristic contraction pattern in a patient with symptoms and signs of ACS but normal coronary arteries on catheter angiography. Cardiac magnetic resonance (CMR), with its latest advancements, is the diagnostic modality of choice for diagnosis, prognosis and follow-up of patients. The advances in CMR (including T1, T2, ECV mapping and threshold-based late gadolinium enhancement (LGE) measurements have revolutionised the role of CMR in tissue characterisation and prognostication in patients with TC. In this review, we highlight the current role of CMR in management of TC and enumerate the CMR findings in TC as well the current advances in the field of CMR, which could help in prognosticating these patients.
Figures




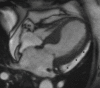
References
-
- Bybee KA, Prasad A, Barsness GW, Lerman A, Jaffe AS, Murphy JG, et al. . Clinical characteristics and thrombolysis in myocardial infarction frame counts in women with transient left ventricular apical ballooning syndrome. Am J Cardiol 2004; 94: 343–6. doi: 10.1016/j.amjcard.2004.04.030 - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

