Mask or no mask for COVID-19: A public health and market study
- PMID: 32797067
- PMCID: PMC7428176
- DOI: 10.1371/journal.pone.0237691
Mask or no mask for COVID-19: A public health and market study
Abstract
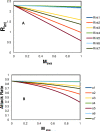
Efficient strategies to contain the coronavirus disease 2019 (COVID-19) pandemic are peremptory to relieve the negatively impacted public health and global economy, with the full scope yet to unfold. In the absence of highly effective drugs, vaccines, and abundant medical resources, many measures are used to manage the infection rate and avoid exhausting limited hospital resources. Wearing masks is among the non-pharmaceutical intervention (NPI) measures that could be effectively implemented at a minimum cost and without dramatically disrupting social practices. The mask-wearing guidelines vary significantly across countries. Regardless of the debates in the medical community and the global mask production shortage, more countries and regions are moving forward with recommendations or mandates to wear masks in public. Our study combines mathematical modeling and existing scientific evidence to evaluate the potential impact of the utilization of normal medical masks in public to combat the COVID-19 pandemic. We consider three key factors that contribute to the effectiveness of wearing a quality mask in reducing the transmission risk, including the mask aerosol reduction rate, mask population coverage, and mask availability. We first simulate the impact of these three factors on the virus reproduction number and infection attack rate in a general population. Using the intervened viral transmission route by wearing a mask, we further model the impact of mask-wearing on the epidemic curve with increasing mask awareness and availability. Our study indicates that wearing a face mask can be effectively combined with social distancing to flatten the epidemic curve. Wearing a mask presents a rational way to implement as an NPI to combat COVID-19. We recognize our study provides a projection based only on currently available data and estimates potential probabilities. As such, our model warrants further validation studies.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures


References
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials

