Prospective Longitudinal Evaluation of Point-of-Care Lung Ultrasound in Critically Ill Patients With Severe COVID-19 Pneumonia
- PMID: 32797661
- PMCID: PMC7436430
- DOI: 10.1002/jum.15417
Prospective Longitudinal Evaluation of Point-of-Care Lung Ultrasound in Critically Ill Patients With Severe COVID-19 Pneumonia
Abstract
Objectives: To perform a prospective longitudinal analysis of lung ultrasound findings in critically ill patients with coronavirus disease 2019 (COVID-19).
Methods: Eighty-nine intensive care unit (ICU) patients with confirmed COVID-19 were prospectively enrolled and tracked. Point-of-care ultrasound (POCUS) examinations were performed with phased array, convex, and linear transducers using portable machines. The thorax was scanned in 12 lung areas: anterior, lateral, and posterior (superior/inferior) bilaterally. Lower limbs were scanned for deep venous thrombosis and chest computed tomographic angiography was performed to exclude suspected pulmonary embolism (PE). Follow-up POCUS was performed weekly and before hospital discharge.
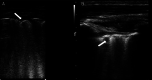
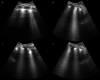
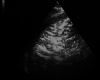
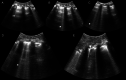
Results: Patients were predominantly male (84.2%), with a median age of 43 years. The median duration of mechanical ventilation was 17 (interquartile range, 10-22) days; the ICU length of stay was 22 (interquartile range, 20.2-25.2) days; and the 28-day mortality rate was 28.1%. On ICU admission, POCUS detected bilateral irregular pleural lines (78.6%) with accompanying confluent and separate B-lines (100%), variable consolidations (61.7%), and pleural and cardiac effusions (22.4% and 13.4%, respectively). These findings appeared to signify a late stage of COVID-19 pneumonia. Deep venous thrombosis was identified in 16.8% of patients, whereas chest computed tomographic angiography confirmed PE in 24.7% of patients. Five to six weeks after ICU admission, follow-up POCUS examinations detected significantly lower rates (P < .05) of lung abnormalities in survivors.
Conclusions: Point-of-care ultrasound depicted B-lines, pleural line irregularities, and variable consolidations. Lung ultrasound findings were significantly decreased by ICU discharge, suggesting persistent but slow resolution of at least some COVID-19 lung lesions. Although POCUS identified deep venous thrombosis in less than 20% of patients at the bedside, nearly one-fourth of all patients were found to have computed tomography-proven PE.
Keywords: COVID-19 pneumonia; acute respiratory failure; chest computed tomography; point-of-care lung ultrasound; pulmonary embolism.
© 2020 American Institute of Ultrasound in Medicine.
Figures





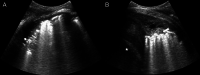
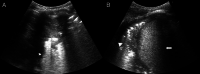
References
-
- Huang Y, Wang S, Liu Y, et al. A preliminary study on the ultrasonic manifestations of peripulmonary lesions of non‐critical novel coronavirus pneumonia (COVID‐19). Social Science Research Network website. 10.2139/ssrn.3544750. [published online February 26, 2020]. - DOI
-
- Buonsenso D, Piano A, Raffaelli F, Bonadia N, de Gaetano Donati K, Franceschi F. Point‐of‐care lung ultrasound findings in novel coronavirus disease‐19 pnemoniae: a case report and potential applications during COVID‐19 outbreak. Eur Rev Med Pharmacol Sci 2020; 24:2776–2780. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

