Drug induced pancreatitis is the leading known cause of first attack acute pancreatitis in children
- PMID: 32800650
- PMCID: PMC7492485
- DOI: 10.1016/j.pan.2020.07.008
Drug induced pancreatitis is the leading known cause of first attack acute pancreatitis in children
Abstract
Background/objectives: Drug induced acute pancreatitis (DIAP) as one of the acute pancreatitis (AP) risks factors is a poorly understood entity. The aim of the current study was to compare the characteristics and course of DIAP cases in children presenting with a first attack of AP.
Methods: Patients presenting with AP were included in a prospective database. We enrolled 165 AP patients that met criteria for inclusion. DIAP patients were included in that group if they were exposed to a drug known to be associated with AP and the rest were included in the non-drug induced-acute pancreatitis (non-DIAP) group.
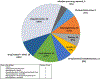
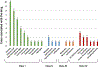
Results: DIAP was observed in 40/165 (24%) of cases, 24 cases had drug-induced as the sole risk factor, and 16 had DIAP with another risk factor(s). The two groups were similar in intravenous fluid and feeding managements, but ERCP was more commonly performed in the non- DIAP group, 14 (11%), vs 0% in the DIAP group, p = 0.02. Moderately severe [9 (23%) vs 11 (9%)] and severe AP [7 (18%) vs 6 (5%)] were more commonly associated with DIAP than non- DIAP, p = 0.001. DIAP was more commonly associated with ICU stay, 10 (25%), vs 12 (10%), p = 0.01, hospital stay was longer in DIAP median (IQR) of 6 (3.9-11) days vs 3.3 (2-5.7) days in non- DIAP, p = 0.001. The DIAP group had a significantly higher proportion of comorbidities (p < 0.0001).
Conclusions: DIAP is a leading risk factor for a first attack of AP in children and is associated with increased morbidity and severity of the pancreatitis course. DIAP warrants further investigation in future studies.
Keywords: Children; Drug induced; Pancreatitis.
Copyright © 2020 IAP and EPC. Published by Elsevier B.V. All rights reserved.
Conflict of interest statement
Declaration of competing interest LAD has received research support unrelated to this work from FrieslandCampina, Glycosyn, and Janssen. SZH has equity in Prevcon, advises for Atias Pharmaceutical, and has received research support from Servier.
Figures
Similar articles
-
Rates and predictors of 30-day hospital readmissions in adults for drug-induced acute pancreatitis: A retrospective study from the United States National Readmission Database.J Gastroenterol Hepatol. 2023 Aug;38(8):1277-1282. doi: 10.1111/jgh.16177. Epub 2023 Mar 30. J Gastroenterol Hepatol. 2023. PMID: 36914611
-
Retrospective Matched-Cohort Analysis of Acute Pancreatitis Induced by 5-Aminosalicylic Acid-Derived Drugs.Pancreas. 2019 Apr;48(4):488-495. doi: 10.1097/MPA.0000000000001297. Pancreas. 2019. PMID: 30946233 Free PMC article.
-
Drug-induced acute pancreatitis: Prevalence, Causative agents, and Outcomes.Pancreatology. 2020 Oct;20(7):1281-1286. doi: 10.1016/j.pan.2020.07.401. Epub 2020 Aug 14. Pancreatology. 2020. PMID: 32878711
-
Drug-Induced Acute Pancreatitis in Adults: An Update.Pancreas. 2019 Nov/Dec;48(10):1263-1273. doi: 10.1097/MPA.0000000000001428. Pancreas. 2019. PMID: 31688589 Review.
-
Recent advances in understanding and managing acute pancreatitis.F1000Res. 2018 Jun 28;7:F1000 Faculty Rev-959. doi: 10.12688/f1000research.14244.2. eCollection 2018. F1000Res. 2018. PMID: 30026919 Free PMC article. Review.
Cited by
-
Clinical and imaging predictors for the development of diabetes mellitus following a single episode of acute pancreatitis in youth.Dig Liver Dis. 2025 Feb;57(2):519-525. doi: 10.1016/j.dld.2024.10.009. Epub 2024 Oct 28. Dig Liver Dis. 2025. PMID: 39462712
-
Current trends in acute pancreatitis: Diagnostic and therapeutic challenges.World J Gastroenterol. 2023 May 14;29(18):2747-2763. doi: 10.3748/wjg.v29.i18.2747. World J Gastroenterol. 2023. PMID: 37274068 Free PMC article. Review.
-
Liberal Fluid Resuscitation is Associated with Improved Outcomes in Pediatric Acute Pancreatitis.J Pediatr. 2025 Jan;276:114329. doi: 10.1016/j.jpeds.2024.114329. Epub 2024 Sep 30. J Pediatr. 2025. PMID: 39357818 Free PMC article.
-
Acute Pancreatitis and Recurrent Acute Pancreatitis in Children: A 10-Year Retrospective Study.Gastroenterol Res Pract. 2022 Jul 22;2022:5505484. doi: 10.1155/2022/5505484. eCollection 2022. Gastroenterol Res Pract. 2022. PMID: 35911080 Free PMC article.
-
Exploring Acute Pancreatitis After Orlistat Use: A Case Report.Cureus. 2025 Mar 19;17(3):e80832. doi: 10.7759/cureus.80832. eCollection 2025 Mar. Cureus. 2025. PMID: 40255727 Free PMC article.
References
-
- Sellers ZM, MacIsaac D, Yu H, Dehghan M, Zhang KY, Bensen R et al. Nationwide Trends in Acute and Chronic Pancreatitis Among Privately Insured Children and Non-Elderly Adults in the United States, 2007–2014. Gastroenterology 155, 469–478 e461, doi:10.1053/j.gastro.2018.04.013 (2018). - DOI - PMC - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

