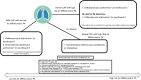
New cephalosporins for the treatment of pneumonia in internal medicine wards
- PMID: 32802454
- PMCID: PMC7399401
- DOI: 10.21037/jtd-20-417
New cephalosporins for the treatment of pneumonia in internal medicine wards
Abstract
The burden of hospital admission for pneumonia in internal medicine wards may not be underestimated; otherwise, cases of pneumonia are a frequent indication for antimicrobial prescriptions. Community- and hospital-acquired pneumonia are characterized by high healthcare costs, morbidity and non-negligible rates of fatality. The overcoming prevalence of resistant gram-negative and positive bacteria (e.g., methicillin-resistant Staphylococcus aureus, penicillin and ceftriaxone-resistant Streptococcus pneumoniae, extended-spectrum β-lactamases and carbapenemases producing Enterobacteriaceae) has made the most of the first-line agents ineffective for treating lower respiratory tract infections. A broad-spectrum of activity, favourable pulmonary penetration, harmlessness and avoiding in some cases a combination therapy, characterise new cephalosporins such as ceftolozane/tazobactam, ceftobiprole, ceftazidime/avibactam and ceftaroline. We aimed to summarise the role and place in therapy of new cephalosporins in community- and hospital-acquired pneumonia within the setting of internal medicine wards. The "universal pneumonia antibiotic strategy" is no longer acceptable for treating lung infections. Antimicrobial therapy should be individualized considering local antimicrobial resistance and epidemiology, the stage of the illness and potential host factors predisposing to a high risk for specific pathogens.
Keywords: Cephalosporins; community-acquired pneumonia (CAP); influenza; methicillin-resistant Staphylococcus aureus (MRSA); multi-drug resistant bacteria; nosocomial pneumonia (NP).
2020 Journal of Thoracic Disease. All rights reserved.
Conflict of interest statement
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/jtd-20-417). FGDR and SC were speaker for Pfizer, MSD and Correvio, FGDR was part of advisory board for Pfizer, MSD. The other authors have no conflicts of interest to declare.