Emergency endovascular treatment of cavernous internal carotid artery acute bleeding with flow diverter stent: a single-center experience
- PMID: 32808087
- PMCID: PMC8195932
- DOI: 10.1007/s00701-020-04517-0
Emergency endovascular treatment of cavernous internal carotid artery acute bleeding with flow diverter stent: a single-center experience
Abstract
Background and objective: To describe our single-center experience in the treatment of cavernous internal carotid artery (ICA) acute bleeding with flow diverter stent (FDS), as a single endovascular procedure or combined with an endoscopic endonasal approach.
Methods: We analyze a case series of 5 patients with cavernous ICA acute bleeding, i.e., 3 iatrogenic, 1 post-traumatic, and 1 erosive neoplastic. After an immediate nasal packing to temporarily bleeding control, patients underwent digital subtraction angiography (DSA) to identify the site of the ICA injury. A concomitant balloon occlusion test (BOT) was performed, to exclude post-occlusive ischemic neurological damage. An FDS was placed with parallel intravenous infusion of abciximab in 3 cases and tirofiban in 2 cases. In two patients, an innovative "sandwich technique" combining the endovascular reconstruction with an extracranial intrasphenoidal cavernous ICA resurfacing with autologous flaps or grafts by endoscopic endonasal approach was performed.
Results: No patient had periprocedural ischemic-hemorrhagic complications. All patients had a regular clinical evolution, without general complications or new onset of focal neurological deficits. No further bleeding occurred in 3 patients, while 2 cases experienced a mild rebleeding in a period ranging from 5 to 15 days after the endovascular procedure. In these two cases, we proceeded with an endoscopic endonasal procedure to resurface the exposed ICA wall in the sphenoid sinus.
Conclusions: Although the treatment of choice for cavernous ICA acute bleeding remains the occlusion of the injured vessel, in cases of poor hemodynamic compensation at the BTO, the endovascular FDS emergency placement can be effective. A combined endoscopic endonasal technique to support the extracranial side of the vessel using autologous flaps or grafts can be performed to prevent the risk of rebleeding.
Keywords: Acute vascular injury; Cavernous carotid artery; Endoscopic endonasal; Flow diverter stent; Hadad flap; Skull base surgery.
Conflict of interest statement
The authors declare that they have no conflict of interest.
Figures

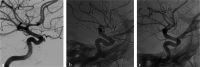


References
-
- Ruiz-Juretschke F, Castro E, Mateo Sierra O, Iza B, Manuel Garbizu J, Fortea F, Villoria F. Massive epistaxis resulting from an intracavernous internal carotid artery traumatic pseudoaneurysm: Complete resolution with overlapping uncovered stents. Acta Neurochir. 2009;151(12):1681–1684. doi: 10.1007/s00701-009-0294-5. - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Miscellaneous

