Decisional Conflict During Major Medical Treatment Decision-making: a Survey Study
- PMID: 32808213
- PMCID: PMC7431116
- DOI: 10.1007/s11606-020-06125-1
Decisional Conflict During Major Medical Treatment Decision-making: a Survey Study
Abstract
Background: Both patients and surrogate decision-makers experience decisional conflict when making a major medical treatment decision with life or death implications. The relationship between health literacy and decisional conflict while making a major medical treatment decision is not understood.
Objective: To identify the prevalence of individuals making major medical treatment decisions for themselves or someone else and to explore the relationships between decisional conflict and circumstances of the decision as well as the decision-maker.
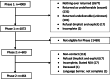
Design: Two-phase survey study: in phase 1, we screened for who made a major treatment decision; in phase 2, we asked eligible respondents about their experience making the decision.
Participants: Address-based random sample of 4000 Wisconsin residents; 1072 completed phase 1 and 464 completed phase 2.
Main measures: We asked respondents about types of decisions made, the most difficult decision made, and characteristics of the decision-maker and the decision. We included the Decisional Conflict Scale and four domains of the Health Literacy Questionnaire. Open-ended questions also allowed respondents to describe their experiences.
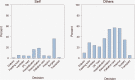
Key results: About 43% of respondents reported making a major medical treatment decision. Decisions about major surgery and life support were regarded as the most difficult decisions. Respondents who made the decision for a spouse/partner (β = 6.65, p = 0.012), parent (β = 9.27, p < 0.001), or someone else (β = 10.7, p < 0.001) had higher decisional conflict. Respondents who reported higher ability to actively engage with healthcare providers (β = - 5.24, p = 0.002) and to understand health information well enough to know what to do (β = - 6.12, p = 0.001) had lower decisional conflict.
Conclusions: The need to make major treatment decisions is likely to increase and making decisions on someone else's behalf appeared to be especially difficult. Improving communication to encourage patient and family engagement in the decision-making conversation, particularly for individuals with limited health literacy, may be helpful.
Keywords: decision-making; decisional conflict; health literacy; survey.
Conflict of interest statement
The authors declare that they do not have a conflict of interest.
Figures
Similar articles
-
Decisions and Decisional Needs of Canadians From all Provinces and Territories During the COVID-19 Pandemic: Population-Based Cross-sectional Surveys.JMIR Public Health Surveill. 2023 Mar 21;9:e43652. doi: 10.2196/43652. JMIR Public Health Surveill. 2023. PMID: 36688986 Free PMC article.
-
People living with chronic pain in Canada face difficult decisions and decisional conflict concerning their care: data from the national DECIDE-PAIN survey.BMC Prim Care. 2024 Dec 19;25(1):424. doi: 10.1186/s12875-024-02667-z. BMC Prim Care. 2024. PMID: 39702110 Free PMC article.
-
Parental decision making involvement and decisional conflict: a descriptive study.BMC Pediatr. 2017 Jun 13;17(1):146. doi: 10.1186/s12887-017-0899-4. BMC Pediatr. 2017. PMID: 28610580 Free PMC article.
-
Decisional Conflict Scale Findings among Patients and Surrogates Making Health Decisions: Part II of an Anniversary Review.Med Decis Making. 2019 May;39(4):315-326. doi: 10.1177/0272989X19851346. Epub 2019 May 29. Med Decis Making. 2019. PMID: 31142205 Review.
-
[Providing insight into the construct decisional conflict and its usability to assess shared decision making].Tijdschr Psychiatr. 2018;60(6):397-402. Tijdschr Psychiatr. 2018. PMID: 29943797 Review. Dutch.
Cited by
-
Associations of Concordant and Shared Lung Cancer Screening Decision Making with Decisional Conflict: A Multi-Institution Cross-Sectional Analysis.MDM Policy Pract. 2025 Jan 17;10(1):23814683241309945. doi: 10.1177/23814683241309945. eCollection 2025 Jan-Jun. MDM Policy Pract. 2025. PMID: 39839686 Free PMC article.
-
Navigating decisional conflict: laser peripheral iridotomy for primary angle-closure glaucoma prevention.Int J Ophthalmol. 2025 Apr 18;18(4):627-636. doi: 10.18240/ijo.2025.04.08. eCollection 2025. Int J Ophthalmol. 2025. PMID: 40256014 Free PMC article.
-
A Video-Based Intervention for Increasing Health Literacy in Total Joint Arthroplasty Patients at a Safety-Net Hospital: A Prospective Single-Blind Cohort Study.Arthroplast Today. 2024 Nov 12;30:101575. doi: 10.1016/j.artd.2024.101575. eCollection 2024 Dec. Arthroplast Today. 2024. PMID: 39619706 Free PMC article.
-
Assessment of a venous thromboembolism prophylaxis shared decision-making intervention (DASH-TOP) using the decisional conflict scale: a mixed-method study.BMC Med Inform Decis Mak. 2023 Nov 6;23(1):250. doi: 10.1186/s12911-023-02349-3. BMC Med Inform Decis Mak. 2023. PMID: 37932759 Free PMC article. Clinical Trial.
-
Path Analysis of Health Literacy, Social Support, and Self-Efficacy on Decisional Conflict in Patients with Stable Schizophrenia.Neuropsychiatr Dis Treat. 2024 Dec 20;20:2571-2583. doi: 10.2147/NDT.S482994. eCollection 2024. Neuropsychiatr Dis Treat. 2024. PMID: 39720413 Free PMC article.
References
-
- American Medical Association. Code of Medical Ethics: Caring for patients at the end of life, 2019, Available at: https://www.ama-assn.org/system/files/2019-06/code-of-medical-ethics-cha.... Accessed Jul 19, 2020.
-
- O’Connor AM. User manual—decisional conflict scale, 2010, Available at: https://decisionaid.ohri.ca/docs/develop/User_Manuals/UM_Decisional_Conf.... Accessed Mar 3, 2020.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

