"Autoinflammatory psoriasis"-genetics and biology of pustular psoriasis
- PMID: 32814870
- PMCID: PMC8027616
- DOI: 10.1038/s41423-020-0519-3
"Autoinflammatory psoriasis"-genetics and biology of pustular psoriasis
Abstract
Psoriasis is a chronic inflammatory skin condition that has a fairly wide range of clinical presentations. Plaque psoriasis, which is the most common manifestation of psoriasis, is located on one end of the spectrum, dominated by adaptive immune responses, whereas the rarer pustular psoriasis lies on the opposite end, dominated by innate and autoinflammatory immune responses. In recent years, genetic studies have identified six genetic variants that predispose to pustular psoriasis, and these have highlighted the role of IL-36 cytokines as central to pustular psoriasis pathogenesis. In this review, we discuss the presentation and clinical subtypes of pustular psoriasis, contribution of genetic predisposing variants, critical role of the IL-36 family of cytokines in disease pathophysiology, and treatment perspectives for pustular psoriasis. We further outline the application of appropriate mouse models for the study of pustular psoriasis and address the outstanding questions and issues related to our understanding of the mechanisms involved in pustular psoriasis.
Keywords: Autoinflammation; Clinical features; Genetics; Histology; IL-36; Pustular psoriasis.
Conflict of interest statement
The authors declare no competing interests.
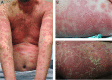
Figures



References
-
- Nestle FO, Kaplan DH, Barker J. Psoriasis. N. Engl. J. Med. 2009;361:496–509. - PubMed
-
- Gudjonsson JE, Elder JT. Psoriasis: epidemiology. Clin. Dermatol. 2007;25:535–546. - PubMed
-
- Gooderham MJ, Van Voorhees AS, Lebwohl MG. An update on generalized pustular psoriasis. Expert Rev. Clin. Immunol. 2019;15:907–919. - PubMed

